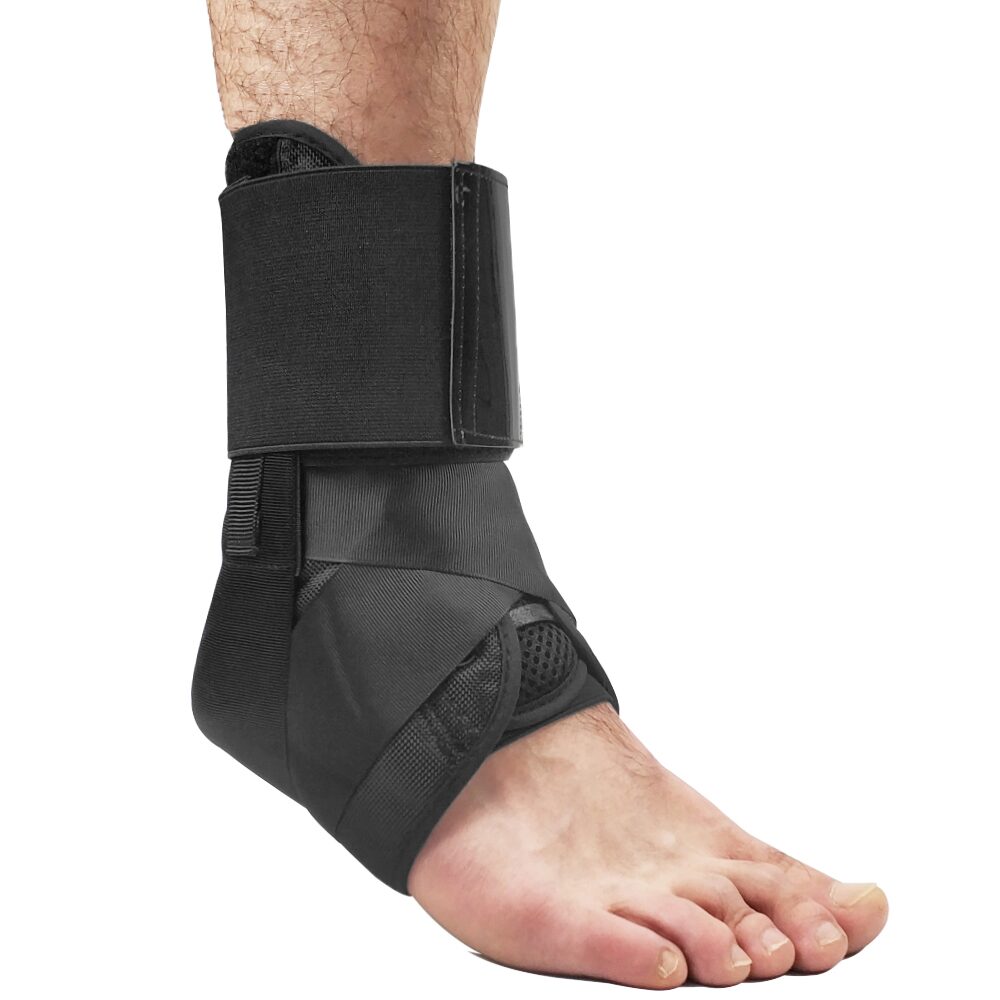
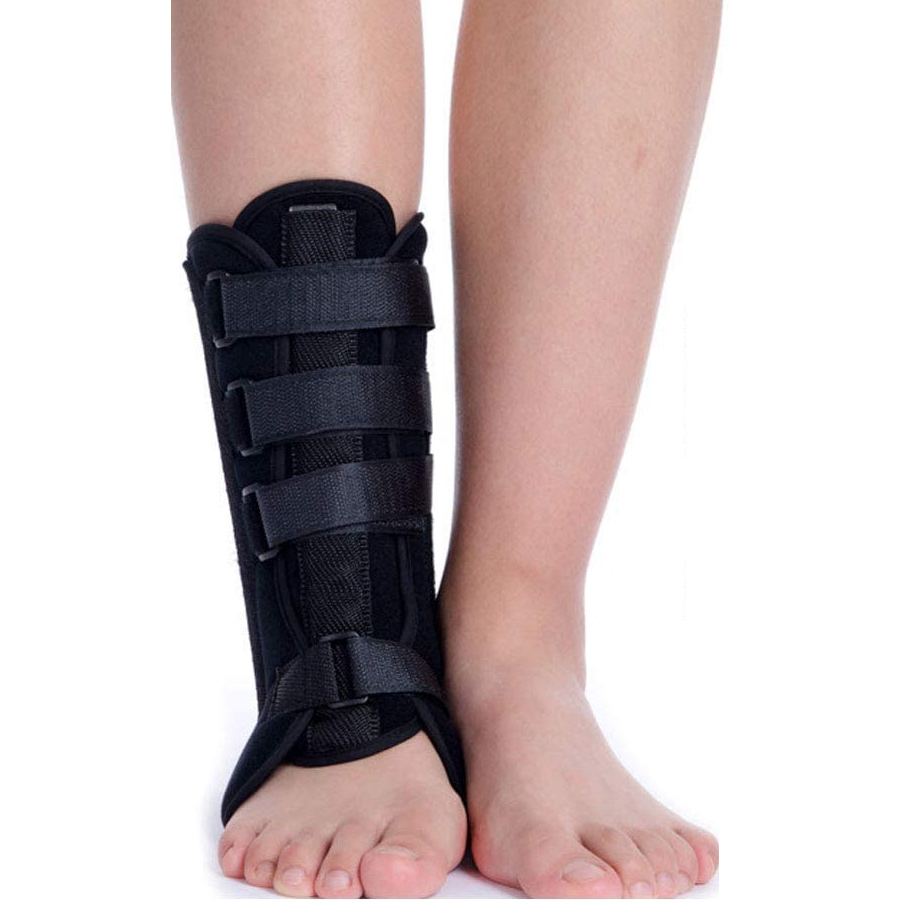
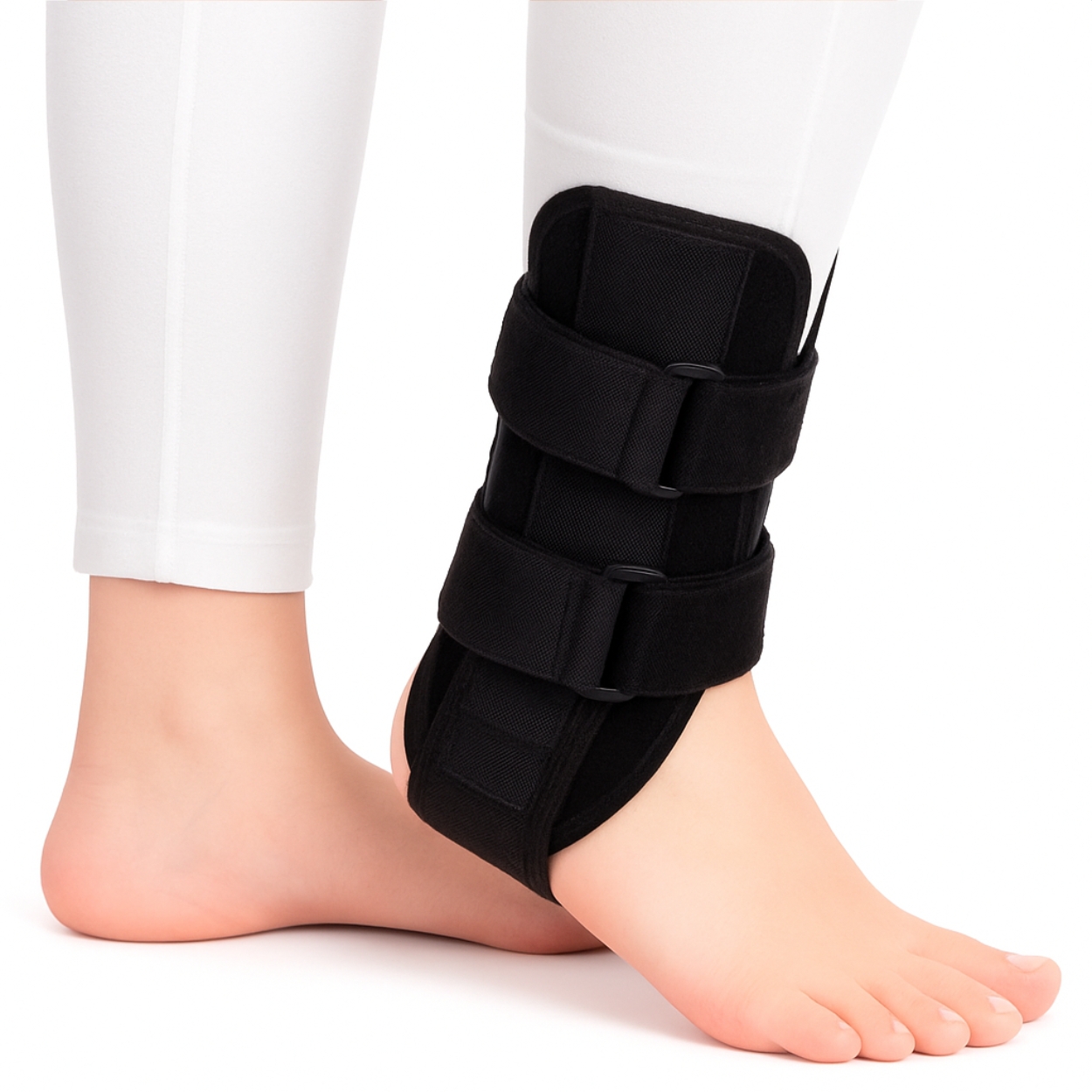
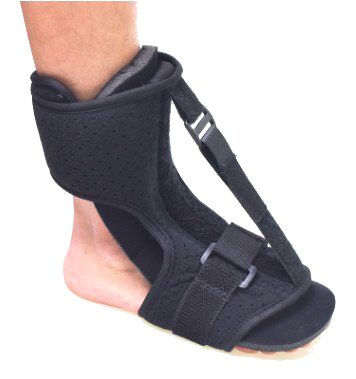
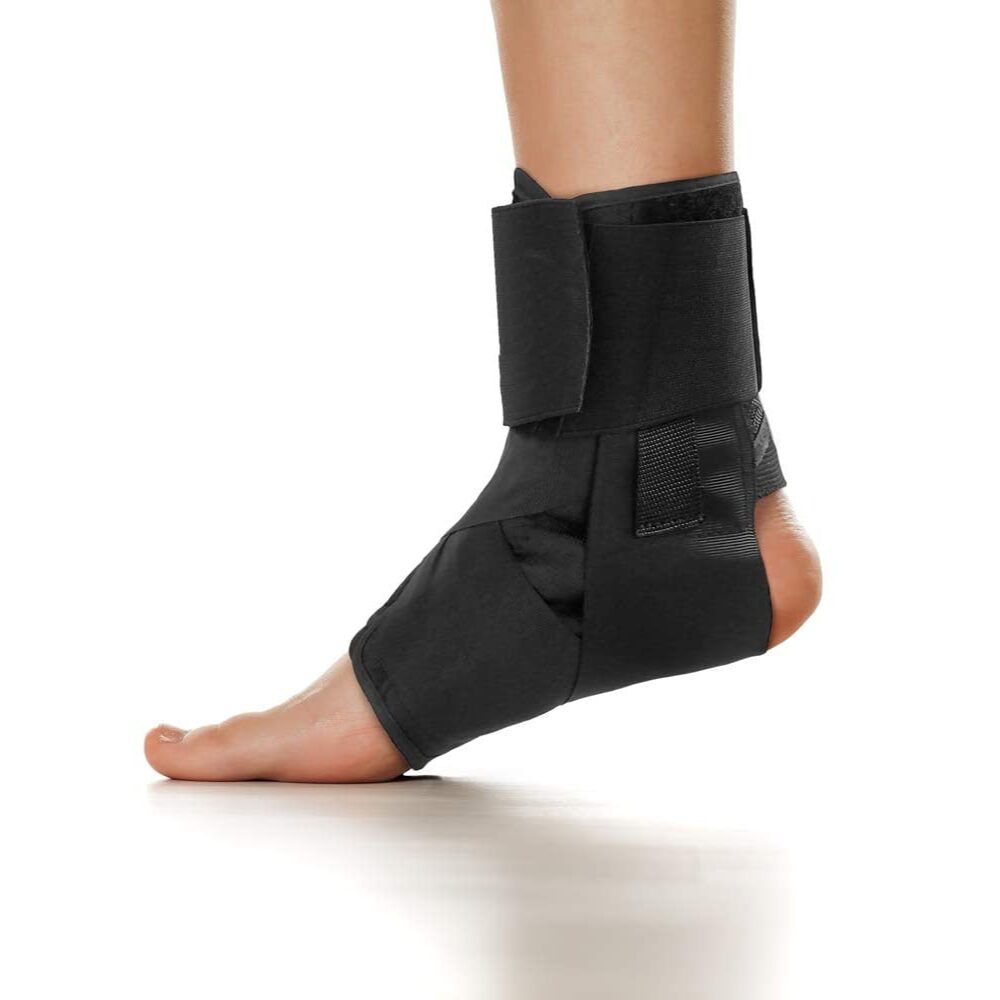
Ankle Splint Foot Brace & Post-Op Cast Support for Ankle Sprains, Fractures, Achilles Tendonitis & Drop Foot
$13.49
$25.63
Living with ankle and foot problemsDo you ever find yourself moving more carefully when your ankle feels sore or unsteady? Having to think about every step soon makes even short walks tiring.In many of these situations, the ligaments, tendons, joints or nerves around the ankle and foot are either recovering from a clear injury or adapting to longer‑term wear, strain or nerve and muscle changes. When these tissues are sore, stretched or not working properly, moving normally or bearing full weight can feel uncomfortable and unstable. A foot‑and‑ankle brace such as this FootReviver design helps by limiting movements that might aggravate the area, supporting the joint, and managing swelling while you focus on recovery and longer‑term management. The aim isn’t to restrict movement but to help you move with more safety and confidence.Muscles in the lower leg control how the foot moves, and their tendons attach to the bones around the ankle and foot. The Achilles tendon, at the back of the ankle, links the calf muscles to the heel bone. It works with every step — helping you push off the ground and lower your heel smoothly. If you walk or run more than usual, or change activity suddenly, small areas within these tendons can become irritated and sore.Under the sole of the foot runs a strong band of tissue called the plantar fascia. It stretches from the heel bone to the toes and helps support the arch. Long hours standing on hard floors, changes in footwear, extra body weight or sudden increases in walking or running can strain this band, especially near its attachment at the heel. This often causes sharp heel pain with the first steps after rest, followed by an ache that builds with activity.Over time, the smooth cartilage covering the ends of the bones can wear down. In arthritis, this cartilage becomes thinner and rougher, and the joint lining can inflame. The ankle may then feel stiff and sore, particularly after rest or long periods of standing or walking.For some people, nerve or muscle problems mean the front of the foot doesn’t lift properly — a condition often called drop foot. The toes can catch on the ground, leading to trips or falls and forcing the leg to lift higher to clear the foot. This can be tiring and place extra strain on other joints.It limits how far and how quickly the ankle rolls or bends into positions that can cause pain or re‑injury. Keeping the joint closer to the middle of its range reduces strain on healing ligaments and on areas already sore.It adds external stability, so the muscles around the ankle don’t have to work as hard to keep the joint centred. This can help if your ankle feels unsteady on uneven ground or after time in a cast when muscles are weaker.It provides gentle, even compression around the ankle and lower leg, helping to reduce swelling and the tightness that often makes movement uncomfortable. When swelling is better controlled, the joint usually moves more freely within a comfortable range.If the front of the foot doesn’t lift fully, holding it closer to a right angle with the lower leg can improve toe clearance as the leg swings forward. This reduces the risk of catching the toes and makes each step feel more secure.A brace doesn’t replace exercises, footwear changes or medical treatment where needed, but it makes those steps easier by giving you a stable, supported joint to build on.What this FootReviver brace is designed to doStructure and alignmentThe FootReviver Ankle Splint Foot Brace & Post‑Op Cast Support is built with a firm frame that surrounds the lower leg and ankle, supported by a stable base under the foot. It reaches to around mid‑calf and, when the front section is attached, it encloses the ankle from all sides for balanced support.Built into the structure of the brace — including the main frame and the detachable front panel — are flexible aluminium splints: two along the outer side of the ankle, two along the inner side, one in the front section, and one running up the back over the Achilles tendon. The side and back splints are pre‑shaped to follow the natural line of the lower leg and ankle, so they rarely need adjustment. The front splint sits in a removable panel that can be gently moulded to follow the front of your shin more closely when you first fit the brace.These splints are firm enough to resist sudden or excessive movement, yet flexible enough to move with you, so the brace feels supportive rather than rigid.The frame and splints are designed to keep the ankle and foot closer to a straight‑ahead position. The side bars help limit the inward roll that often leads to sprains on the outer side of the ankle, and the outward roll that strains the inner side. The front and back bars add control to forward and backward bending at the ankle while still allowing you to walk naturally. Because the brace extends to mid‑calf, it takes control from higher up the leg, giving the splints more leverage to resist unwanted motion and spreading pressure over a larger area for comfort. The frame and strap layout reflect how ankles typically sprain and recover, based on what physiotherapists and podiatrists observe in daily practice. By guiding the joint through a safer range as you stand and walk, the brace helps protect healing ligaments and reduce pressure on irritated joint surfaces.Straps and adjustabilitySeveral buckled straps run across the foot, around the ankle, and up the lower leg. These allow the brace to fit closely around your leg so it moves with you rather than slipping or rubbing.Because each strap is anchored in a different position on the brace, you can adjust them independently to suit your comfort. You might prefer firmer support around the ankle joint when walking longer distances, and slightly gentler tension when moving around the house. This flexibility helps you match the level of support and compression to your activity and to changes in swelling through the day. The strap layout is designed so most people can manage it themselves or with minimal help.Compression and swelling controlThe brace provides steady, comfortable compression around the ankle and foot. This gentle pressure helps limit swelling and can ease the feeling of heaviness or tightness that often builds by the end of the day.When swelling is better controlled, the ankle usually has more room to bend and straighten within a comfortable range. This makes early movement easier when the joint feels stiff and supports the goal of combining protection with gradual return to activity, as advised by your doctor or therapist.Positioning and movementOne of the main functions of this brace is to hold the foot closer to a right angle with the lower leg and to control side‑to‑side roll. The flexible splints along the sides, front, and back help resist sudden twists or extreme bending while still allowing normal walking movements. This reduces strain on tissues that are sensitive to sudden or excessive movement.If your ankle tends to roll inwards after a sprain, the side supports in this FootReviver brace help resist that roll. If you have had sprains before or feel your ankle might give way, this positioning helps reduce sudden inward or outward twists, especially on uneven or sloping ground. After fractures or time in a cast, the splints and frame can make the ankle feel more stable when you first return to normal weight‑bearing. In drop foot, holding the foot up helps the toes clear the ground more easily and may reduce tripping. The rear splint over the Achilles area also helps limit strong downward pointing of the foot, which can be uncomfortable when the tendon or post‑surgical area is sensitive, while still allowing a normal push‑off during walking.Comfort and wearabilityThe brace is made from lightweight, breathable materials and has a slim profile. Air can circulate around the skin, and moisture is less likely to build up compared with heavier, enclosed boots. Padding around the ankle bones and heel helps spread pressure and reduce rubbing over these bony points, especially when the brace is worn for longer periods. This helps lower the risk of skin irritation when you spend long hours on your feet.Because it is not bulky, many people can wear it inside suitable footwear such as trainers or walking shoes with extra depth and adjustable fastenings. Being able to use the brace in everyday shoes, once your doctor or therapist confirms it is appropriate, means you can benefit from its support at home, outdoors, and at work. Many people, and the clinicians who support them, value that this brace fits into common footwear rather than requiring a separate, rigid boot.Durability and careThe brace is designed for regular use during recovery and for ongoing support when needed. The frame and straps are made to withstand daily use and the normal movements of walking and standing.It is still worth checking it from time to time. Look for any fraying straps, loose stitching, or fastenings that no longer hold securely. Wipe the brace if it becomes damp with sweat, allow it to air dry away from direct heat, and make sure it is fully dry before wearing it again. These steps help keep it comfortable and in good condition.Getting the fit rightChoosing a sizeThis brace comes in three sizes based on UK shoe size:Small: UK 3–5Medium: UK 5–8Large: UK 8–11Choosing the correct size is important. A brace that is too small may dig in, cause sore spots, or restrict circulation. One that is too large may not control movement properly and could slip. If you are between sizes, know that your foot tends to swell, or are unsure, it is worth checking with a doctor, physiotherapist, or podiatrist familiar with your ankle and foot. Also consider the socks or clothing you plan to wear under the brace. The design is universal, so the same brace can be worn on either the left or right foot as long as the size is correct.If you are between sizes, think about how much your foot and ankle usually swell and whether you plan to wear a thicker or compression sock. In borderline cases, a slightly larger brace may feel more comfortable, provided the straps can still be tightened enough to control movement.Putting the brace onTo get the most benefit, position the brace correctly before tightening the straps. Your heel should sit right back in the heel section, and your foot should rest flat on the base so the ankle sits roughly at a right angle.Fasten the straps starting near the ankle joint, then move up the leg and along the foot. Each strap should feel firm enough to give support but not so tight that it causes pain, pins and needles, or changes the colour of your toes. The first few times you use the brace, it may take a few attempts to find the most comfortable and secure fit, especially if your ankle is still swollen. Many people find it easier once they have seen it fitted step by step.The front panel can be gently shaped to follow the front of your shin more closely before tightening the straps over it. It is usually best to wear a thin or compression sock under the brace to protect the skin and improve comfort, as long as the brace and footwear still fit without feeling tight. Ensure that the straps are looped fully through the buckles. Slip your foot through the brace whilst placing the detachable splint onto the front of your foot/lower leg. Tighten the Velcro straps to the appropriate fit and compression that you need Make sure that the ankle brace fits correctly and securely. Make sure that the brace is not too tight and does not restrict blood flow to your footHow it should feelWhen the brace fits well, your ankle should feel more secure, especially in the directions that previously felt weak or painful. You should notice a firm, even hold around the joint rather than sharp pressure in one spot. Your toes and the part of your foot beyond the brace should stay warm, with normal sensation.You should still be able to move your ankle within the safe range your doctor or therapist has advised for your stage of recovery. At first, the brace may feel slightly unfamiliar because it guides your movement differently. Most people adjust to this quickly. If the brace digs in, slips, or fails to limit the movements that cause discomfort or instability, the fit or size may need to be checked.Common fitting problems and checksIf your heel is not fully seated at the back of the brace, the ankle will not be held securely and rubbing is more likely. Straps that are much tighter in one area than another can also create pressure points. After wearing the brace for a few minutes while standing or walking, check how it feels and make small adjustments if needed.If your ankle and foot tend to swell at certain times, such as later in the day, you may need to loosen or re‑tighten the straps slightly. Persistent redness after removing the brace, blisters, sore spots, or new numbness or tingling are signs to contact a doctor, physiotherapist, or podiatrist for review.How and when to use the brace day to dayEarly after injury or surgeryIn the first days and weeks after a sprain, fracture, or operation, the main aim is to protect healing tissues. During this stage, your doctor or therapist will usually set clear limits on how much weight you can place through the foot and how far you can move the ankle.If a brace like this is recommended, you may be asked to wear it whenever you are standing or walking. It helps keep the ankle in a safer position and provides extra support as you begin to put weight through it again. The brace can also help you move from a rigid cast or boot towards more natural walking. It should not be used to exceed any weight‑bearing or activity limits set by your medical team.Rehabilitation phaseAs pain and swelling settle and movement becomes easier, the focus usually shifts to rebuilding strength, flexibility, and control. During this phase, the brace can still be useful as you start to increase your activity.You may be advised to wear it for longer walks, uneven ground, or exercises that challenge your balance. In safer situations, such as controlled exercises on flat ground or short tasks at home, you might spend short periods without it so your muscles and joint can begin to manage without constant external support. The right balance between time with and without the brace depends on your progress, and your physiotherapist or doctor can guide you on when to rely on it and when to practise short spells without it.Long‑term use for instability and arthritisFor ongoing issues such as chronic instability or ankle arthritis, the brace can play a part in day‑to‑day management. Many people choose to wear it on days when they expect to be more active, when symptoms are worse, or for tasks that usually bring on pain or a sense that the ankle might give way.On days when you are doing less or only short, low‑demand activities at home, some people manage without the brace, using supportive footwear, any recommended insoles, and planning how they spread activity through the day. How often you use the brace and in which situations is best decided with a doctor, physiotherapist, or podiatrist who understands your ankle and overall health.Sport and higher‑risk activitiesWith your medical team’s agreement, the brace can sometimes be worn during sports or activities that involve running, jumping, or quick changes of direction. Its structure and strap system can help reduce the risk of a sudden roll or twist in these situations.The brace is not designed for unrestricted, high‑impact twisting sports or very deep ankle movements until your doctor or physiotherapist confirms you are ready. It should be seen as added protection within a gradual return to activity, not as a substitute for rehabilitation. A safe return to sport depends on healed tissues, good strength and control, and a steady increase in training load. The brace supports that process rather than replacing sport‑specific recovery work.When to wear it and when to take it offMost people wear this type of brace when they are on their feet, bearing weight, or doing activities that test balance or stability. When resting with your leg raised, or sitting or lying for longer periods, there is usually less need for the brace, and it can help your skin and soft tissues to have some time without pressure.For most people, that includes overnight. This type of brace is not normally intended for sleeping unless your specialist has specifically advised it. At night, your ankle is not taking weight, and the skin and circulation benefit from a break from straps and compression. This is particularly important if you have diabetes, circulation problems, a history of blood clots, or reduced sensation in your feet.Wearing any brace for very long periods without breaks, especially if you are not moving much or overnight, can increase the risk of rubbing and pressure problems. This is especially relevant for people with reduced sensation or known circulation issues, such as some with diabetes. If you use compression socks or insoles with the brace, make sure your footwear is not too tight around the foot and ankle, as this can restrict blood flow. If you are unsure, check with a doctor or other health professional. Unless you have been clearly advised to wear it at night or for extended periods, it is usually best to remove the brace at intervals, check your skin, and allow the area to air before putting it back on.Who this brace is suitable forWhen this brace is often usedThis ankle–foot brace is commonly used for:Support during recovery after ankle sprains and strains, once a serious injury has been ruled out. It helps stabilise the joint while the ligaments and soft tissues recover, reducing the risk of another twist during early movement.Extra protection and reassurance after fractures, when a doctor or specialist recommends moving from a cast or boot into a brace. It provides controlled support as you start to bear weight again, helping the ankle adjust gradually to normal activity.Ongoing instability, when the ankle feels as if it may give way, especially on uneven or sloping ground. The brace limits excessive side‑to‑side movement and gives a firmer sense of control when walking or standing for longer periods.Problems affecting the Achilles tendon and other tendons around the ankle. By reducing strain on these tendons, the brace can make walking and gentle exercise more comfortable while healing continues.Flare‑ups of heel or arch pain linked to the plantar fascia, by improving how the ankle and foot move during walking. Supporting the ankle in a more neutral position can ease tension through the arch and reduce irritation where the fascia attaches to the heel.Ankle arthritis, to ease some of the mechanical stress, particularly during longer walks or periods of standing. The brace helps share the load more evenly across the joint, which can make movement smoother and less painful.Drop foot, to improve walking safety when lifting the front of the foot is difficult, under specialist guidance. It helps keep the foot in a safer position during each step, reducing the risk of tripping and improving confidence on uneven ground.The post‑operative phase, to provide extra protection when this has been recommended by the treating team. It supports the ankle and foot as tissues heal and strength returns, helping you move more safely during recovery.Many people with these problems also find it helpful to use supportive or shock‑absorbing insoles or heel lifts, such as those available in the NuovaHealth range, alongside the brace where shoe space allows. With the right fitting and advice, most people find this type of brace comfortable and straightforward to use.When to speak to a clinician before using itIf you have recently injured your ankle or foot and have very severe pain, notice that the joint looks out of place, cannot put any weight at all through the foot, or develop very rapid swelling, you should seek urgent medical assessment before using a brace. These signs can indicate a fracture or another serious injury that needs specific treatment rather than simple support.If you notice sudden new weakness, marked numbness or tingling, or changes in skin colour or temperature in the foot, these can signal problems with circulation or nerve function, so it’s best to speak to a doctor promptly. In conditions such as drop foot, assessment by a doctor and, where appropriate, a specialist service is important to understand the cause and consider all treatment options.When this brace is an extra, not the main treatmentIn conditions such as plantar fascia‑related heel pain or ankle arthritis, other measures usually do most of the work. These might include supportive footwear, insoles to help position the foot, exercises to improve strength and flexibility, spreading activity more evenly through the day, weight management, and medicines where needed. These approaches target the underlying causes of strain and stiffness, helping to improve long‑term comfort and mobility.In these situations, an ankle–foot brace can still be useful as extra support in particular circumstances, such as during flare‑ups or for tasks you know tend to bring symptoms on. It is unlikely to be the only or main treatment, but it can make a noticeable difference when symptoms increase or activity levels rise. A doctor, physiotherapist, or podiatrist can advise you on how best to combine bracing with these other approaches. If you are already using compression socks or insoles as part of your care, they can also advise on how best to combine them with this brace.Special situationsPeople with conditions that affect circulation, skin health, sensation in the feet, or wound healing need to take extra care. If you have open wounds, fragile skin, reduced sensation in the foot or leg (for example due to diabetes or other nerve problems), or known circulation problems, it is especially important to speak to a doctor or specialist before using a brace that applies compression and covers a large area of skin.In these cases, careful fitting, shorter initial wear periods, regular skin checks, and clear advice on how long to wear the brace at a time are all important. Your clinician can help you decide if this brace is suitable for you, when to wear it, and what early warning signs to watch out for.More detail on common ankle and foot problemsThe sections below give more detail on ankle and foot problems where this type of brace is often used. If one of these descriptions sounds similar to your experience, you can open that section to read more about what may be happening and how the brace can play a part in managing it.Ankle sprains – protecting ligaments while they healWhen an ankle sprain happens, there’s usually a single moment that stands out. It might be landing on the outer edge of the foot, stepping into a dip you didn’t see, or turning quickly and feeling the ankle roll inwards. Pain is usually sharp at the moment of injury. Swelling builds over the next few hours, and putting weight on that foot can feel very difficult. Bruising often appears around the outside or front of the ankle within the first few days.Most sprains affect the ligaments on the outer side of the ankle, particularly the anterior talofibular ligament, which connects the lower end of the fibula to the talus bone in the foot. When the sole of the foot turns inwards and the outer edge drops towards the ground, this ligament is stretched beyond its normal range. The calcaneofibular ligament, which runs from the fibula to the heel bone, can also be strained in the same movement. These ligaments act like firm straps that limit how far the ankle joint can tilt or roll. When they’re overstretched or partly torn, small blood vessels in the surrounding tissue can also tear, leading to local bleeding and swelling. The damaged tissue releases inflammatory substances that irritate nearby nerve endings, which is why the area becomes painful and tender to touch.In the first few days, local blood flow increases and inflammatory fluid builds up around the injured tissue as part of the body’s repair process. This natural response helps clear damaged fibres and begin repair, but it also makes the ankle feel full, hot, and tight. Movements that stretch the injured ligaments — especially turning the foot inwards or bearing full weight on that leg — can cause sharp pain because the healing fibres aren’t yet strong enough to resist tension. At this stage, the tissue is fragile, and another sudden inward roll of the foot can easily reopen the injury.Once the initial swelling and pain begin to settle, gentle movement and controlled support become key to regaining confidence in the ankle. Over the next few weeks, the torn fibres knit together and gradually remodel into stronger tissue. Swelling and bruising fade, but many people still notice that the ankle feels weak or “not right”, particularly when walking on uneven ground or changing direction quickly. The ligaments may not yet have regained their normal tension, and the ankle’s position sense — the feedback from small receptors in the ligaments and muscles that tell the brain where the joint is — is often dulled after a sprain. This reduced awareness makes it harder for the muscles around the ankle, such as the peroneal muscles on the outer side of the lower leg, to react quickly when the foot starts to roll. As a result, the joint can still feel unstable even after pain and swelling have eased. The muscles that stabilise the ankle may also have lost some strength and coordination, which adds to the sense of unsteadiness.A structured brace can be especially helpful during this stage of recovery. By holding the ankle in a neutral position — with the sole of the foot flat and the heel aligned beneath the leg — the FootReviver brace limits how far the ankle can roll inwards or outwards. This reduces strain on the healing ligament fibres and helps prevent sudden, uncontrolled movements that could cause another sprain. The brace also provides gentle compression around the joint, which helps limit fluid build‑up during the day. Better control of swelling often means less tightness and throbbing towards the end of the day. When the ankle feels more contained and supported, it’s easier to move it gently within the safe range your doctor or physiotherapist has advised. These early, comfortable movements are important for preventing stiffness and helping the new ligament fibres align in the right direction as they strengthen.As the weeks go by, the way the brace is used usually changes. In the early stages it may be worn for most standing and walking, following your medical team’s advice. Once pain and swelling have eased and you’ve started rehabilitation exercises, many people move towards using the brace for higher‑risk situations — for example, longer walks, walking on uneven ground, or early practice for a chosen sport. At the same time, exercises that focus on balance, strength, and joint control help the ankle muscles take back more of the stabilising work. With consistent use and gradual exercise, most mild to moderate sprains improve steadily over several weeks, but full recovery of strength and balance can take longer, which is why ongoing support and exercise are important.If, after a twist, you can’t put any weight at all on the foot, if the ankle looks clearly out of place, or if pain and swelling are severe and continue to worsen, it’s important to seek urgent medical assessment before using a brace. These features can indicate a fracture or a more serious injury that needs specific treatment rather than simple support.Recurrent weak ankles and instabilityMany people describe having “weak ankles” for years. It is rarely one major injury, but more often a series of smaller twists and stumbles that happen more often than they should. You might notice yourself tensing up on rougher paths, feeling uneasy on slopes, or avoiding walking quickly because you are unsure how the ankle will cope. Even if pain is not constant, the sense that the joint could give way at the wrong moment can be draining.This longer‑term instability often begins with one or more significant sprains in the past. When ligaments are stretched or partly torn, they may heal in a slightly lengthened position. The joint then depends more on the surrounding muscles and the body’s position sense to keep it centred. The muscles on the outer side of the lower leg, particularly the peroneal group, play a key role in preventing the ankle from rolling inwards. When these muscles are slow to react or weaker after repeated sprains, the joint becomes more vulnerable to further twists. If those systems do not fully recover, small wobbles are not corrected as quickly or as precisely as before. Over time, that leaves the ankle more likely to roll again, even with relatively minor triggers.When your sense of where the ankle is in space is reduced, the body’s reflexes respond more slowly as it starts to tilt — which is why small slips can so easily turn into full twists. Because of this, many people unconsciously change how they move. Some keep the ankle unusually stiff, others shift more weight through the opposite leg, and some avoid uneven or sloping routes whenever possible. These adjustments help prevent mishaps in the short term but may lead to extra strain higher up the leg or in the lower back. Mentally, always scanning the ground and thinking about your ankle with every step can be tiring — and that is a very common experience.Instability tends to stand out in certain situations. Walking on soft or uneven ground feels uncomfortable because the ankle has to adapt to constant small changes in surface. Going down slopes or steps can be unsettling when the ankle feels as if it might roll as your weight moves forwards. Carrying bags or loads adds to the worry, as you cannot always see exactly where your foot is landing.In these situations, an ankle–foot brace provides reliable support and stability. The FootReviver brace supports the ankle in a straighter position and limits how far it can suddenly roll inwards or outwards. That extra control makes walking across uneven ground, tackling slopes, or moving through crowded areas feel more predictable. The gentle but firm contact around the joint also improves awareness of where your ankle is, helping your body fine‑tune its control with each step. As confidence returns through a mix of support and retraining, many people find they can move more naturally again without constantly thinking about each step.Many people with long‑standing instability use a brace selectively rather than all the time. It is often worn for higher‑demand situations — longer walks, days with more time on your feet, or light sport and exercise where a twist would have bigger consequences. On shorter, flatter walks or at home, some find they can manage without it, especially as strength and control improve.A brace works best alongside exercises that target ankle stability. These might include balance work on one leg, controlled movements that take the ankle gently towards less comfortable positions, and strengthening exercises for the muscles around the ankle and hip. Used together, the brace provides support and reassurance when you are out and about, while the exercises help the joint and surrounding muscles gradually take back more of the stabilising work themselves.If, despite appropriate exercises and sensible brace use, the ankle continues to give way frequently, or if you notice deep joint pain, catching, or a feeling that something is blocking movement inside the ankle, it is sensible to ask for further assessment. In some cases, there may be cartilage or joint surface changes that need specific investigation and advice.Achilles tendon problemsPain or stiffness at the back of the ankle or just above the heel is often linked to the Achilles tendon. Many people find it is most noticeable first thing in the morning or when getting up after sitting for a while. The first few steps can feel tight or sore, as if the tendon needs to warm up. As you move around, it may ease for a time, then ache again later in the day or after a longer walk. This type of tendon pain usually develops gradually rather than from a single injury.The Achilles tendon connects the calf muscles to the heel bone and helps control how your heel lifts off the ground and how you push forwards with each step. With walking, running, or repeated stair use, the tendon is constantly being loaded and then allowed to relax. Tendons adapt more slowly than muscles to changes in activity, so when load increases too quickly, the tissue becomes irritated before it has time to strengthen. These irritated areas may thicken and become more sensitive, which is why the tendon feels stiff and sore. Overnight, blood flow through the tendon slows, which is why stiffness is often most noticeable first thing in the morning.Certain movements and tasks place particular demand on the Achilles. Walking or running uphill makes the calf work harder to lift the body, increasing the pull through the tendon. Going downstairs or down slopes asks the tendon to control the lowering of the heel as your weight moves forwards and down. Pushing off quickly — for example, to sprint or change direction sharply — places a sudden high load on the tendon as it stores and releases energy. Footwear with very flat soles or poor cushioning increases strain by forcing the tendon to stretch more with each step. When the tendon has been sore for a while, it is common to feel cautious with these movements. It can seem as though every slope or set of stairs needs to be approached carefully.An ankle–foot brace plays a useful part in managing these problems by changing how the ankle moves during the tasks that challenge the tendon. By supporting the ankle within a controlled range and reducing how far it bends forwards over the foot, the brace limits how much the Achilles stretches with each step. This is particularly helpful on slopes, stairs, or longer walks, where repeated deep bending at the ankle tends to aggravate symptoms.The brace also adds stability around the ankle. When the joint feels more secure, it is often easier to take smoother, more predictable steps rather than sudden, guarded, or uneven movements. That reduces the risk of jerky, inconsistent loading through the tendon that might otherwise irritate sensitive areas. Some people find that using the brace for specific tasks — such as hill walking, longer outings, or the early stages of returning to running — makes those activities more manageable.This support works best alongside other measures. Stretching and strengthening exercises for the calf and ankle, gradual adjustment of training load, and attention to footwear all have important roles. The brace fits into that picture by helping you manage certain walking or exercise demands while you work on the underlying strength and control.If you experience a sudden, severe pain in the area of the Achilles tendon — especially if it feels as though you have been kicked at the back of the ankle, hear or feel a snap, and then find it hard or impossible to push up onto your toes — you should seek urgent medical assessment. These features suggest a more serious tendon injury that needs prompt, specific treatment.Plantar fascia‑related heel and arch painHeel pain that feels sharp with the first few steps in the morning, or after sitting for a while, is often linked to the plantar fascia – the strong band of tissue running along the sole of the foot. Many people describe a stabbing pain under the heel when they first stand up. As they move around, the pain often eases to a dull ache, only to build again after longer periods of standing or walking.The plantar fascia runs from the heel bone towards the toes and acts like a tensioned spring that supports the arch of the foot. Each time you stand or take a step, it tightens as your heel lifts and relaxes as your foot leaves the ground. When this band is repeatedly strained, small areas near where it attaches to the heel bone can develop tiny tears and local inflammation. During rest, the tissue cools and stiffens slightly. When you stand again, those first few steps stretch an already sensitive area, which is why the early pain can be so sharp.Several factors can increase strain on the plantar fascia. Long hours standing on hard floors, a sudden increase in walking or running, shoes with poor arch support or very thin soles, extra body weight, and tight calf muscles can all contribute. When the arch flattens more than usual with each step, the fascia stretches more, especially near the heel. Over time, repeated small overloads can lead to ongoing irritation and stiffness. This pattern, particularly when it continues for months, can be tiring and discouraging.Managing plantar fascia‑related pain usually involves several steps working together. Footwear with good cushioning and support helps reduce repeated stress on the fascia. Insoles or orthoses can support the arch and spread forces more evenly through the foot. Stretching and strengthening exercises for the calf and foot muscles help those tissues share the load more effectively. Adjusting activity levels, especially around long periods of standing or higher‑impact exercise, is often important. Improvement tends to come gradually as the tissue adapts and settles, so consistency matters more than speed.An ankle–foot brace is not usually the first treatment for plantar fascia problems, but it can play a useful supporting role in some situations. By helping to control how the ankle moves, the brace influences how the foot lands and rolls during walking. Limiting excessive inward or outward rolling of the ankle can, for some people, reduce the extra stretch placed on the fascia with each step, particularly when walking on uneven ground or over longer distances.The brace also provides stability and gentle compression around the ankle and foot. This can make it easier to take more even, controlled steps at times when pain would otherwise cause you to limp or favour one side. During flare‑ups, using the brace for specific tasks that usually bring symptoms on – for example, longer walks or days with more standing – can help keep discomfort at a manageable level while other treatments do their work.Because plantar fascia‑related pain often has several contributing factors, it is worth discussing with a clinician how an ankle–foot brace fits into your overall care. They can help you decide when bracing is appropriate, how often to use it, and how best to combine it with footwear changes, insoles and exercises.If heel pain is accompanied by marked swelling, redness, warmth, or follows a direct injury that makes it difficult to bear weight, medical assessment is advisable to rule out other causes such as a fracture or infection.Ankle arthritis and longer‑term stiffnessAnkle arthritis often develops gradually. Many people notice the ankle feels stiff and awkward when they first get up or after sitting for a while. It may ease a little as you start walking, only to become more achy or sore if you are on your feet for a long time. Some days the joint feels reasonably settled; on others it can feel heavy, swollen or difficult to move without a clear reason. The mix of better and worse days makes planning ahead difficult, and that unpredictability itself can be a source of stress.In ankle arthritis, the smooth cartilage that covers the ends of the bones becomes thinner and less even. The lining of the joint can also become irritated and produce extra fluid. As cartilage wears away, the underlying bone is exposed and can become sensitive, adding to the aching and stiffness. The surrounding muscles may tighten or weaken over time, which can make the joint feel even less mobile. When you move or put weight through the ankle, certain parts of the joint come under more pressure than they can comfortably handle, especially when the joint is taken towards the end of its range.There are several types of arthritis that can affect the ankle. The most common is osteoarthritis, where gradual wear of the joint surfaces follows previous injury or long‑term mechanical stress. Inflammatory types, such as rheumatoid arthritis, psoriatic arthritis, or ankylosing spondylitis, involve the body’s immune system attacking the joint lining, leading to swelling, warmth, and stiffness that can fluctuate. Post‑traumatic arthritis develops after a significant ankle injury, such as a fracture or severe sprain, when the joint surfaces have been damaged. Less commonly, crystal‑related arthritis (such as gout) can cause sudden, intense pain and swelling. Each type affects the joint in slightly different ways, but the result is similar — the ankle becomes less smooth, less flexible, and more prone to aching and stiffness with use.Activities that keep you on your feet for long periods often bring symptoms out. Standing in one place for too long, walking longer distances on hard surfaces, or going up and down slopes can all increase ache and swelling. Walking on uneven paths can also be difficult, because the ankle has to adjust constantly to small changes in position. In these situations, many people find themselves moving more cautiously or planning routes carefully to avoid too much discomfort.Movements at the far ends of the ankle’s range tend to be more uncomfortable. Deeply bending the ankle forwards over the foot, or pointing the foot strongly down, can squeeze or irritate sensitive parts of the joint surface. Many people with ankle arthritis naturally avoid these extremes. While that helps reduce pain, completely avoiding movement can, over time, add to stiffness and make the joint less adaptable.An ankle–foot brace can help by limiting movement into the positions that cause the most discomfort. By holding the ankle closer to a mid‑position and reducing excessive twist and bend, the brace reduces pressure on sore joint surfaces when you stand and walk. Keeping the joint in a straighter alignment helps weight spread more evenly across the ankle, rather than concentrating force on one small, painful area. Less concentrated load often means less end‑of‑day aching and a steadier, more comfortable stride.The brace also provides a sense of support around the ankle. When the joint feels more secure, it is easier to take smoother, more confident steps instead of moving very cautiously or with a stiff gait. That smoother movement can reduce the extra effort that sometimes shows up as aching in the lower leg or higher up the chain. By improving alignment and control, the brace can also help conserve energy during longer periods on your feet.Many people with ankle arthritis use a brace on an “as needed” basis. It may be particularly helpful on days when more walking or standing is expected, or during phases when the joint feels more unsettled and swollen. On quieter days, or for very short trips, some manage without bracing, relying more on supportive footwear and pacing their activities. A doctor or physio can help you decide when using the brace is most worthwhile for your ankle.The brace is one part of an overall approach to managing ankle arthritis. Medicines, exercises to keep the joint moving and the surrounding muscles strong, weight management where relevant, and occasionally other medical interventions all play important roles. The brace’s job is to support the joint mechanics during weight‑bearing, not to change the underlying joint condition. Keeping the ankle moving within a comfortable range and maintaining strength around it can help slow stiffness progression and preserve mobility.If your ankle becomes suddenly much more painful, if swelling increases quickly, or if the joint feels hot, red or is associated with fever or feeling generally unwell, you should seek medical assessment. These features can indicate a problem such as infection or a new fracture and need prompt attention.Fractures, post‑op and post‑cast protectionWhen a cast or walking boot comes off after an ankle or foot fracture, or after surgery in that area, those first steps can feel unfamiliar. The ankle often feels stiff and heavy, and the leg may seem weaker than expected. You might be unsure how much weight is safe to put through the foot. Even simple things like standing up from a chair or walking across a room can feel like a big effort at first.This is completely normal. While the ankle or foot has been immobilised, the bones and soft tissues have been protected so they can heal, but the muscles have not been working as they usually would. They lose strength and bulk, and the joint becomes less flexible. The small sensors in and around the joint that help with balance and position sense are also less active. Even when X‑rays show good healing and your medical team are happy with progress, the muscles, tendons and balance systems still need time to catch up. Feeling cautious at this stage is a natural response to that temporary weakness.These issues are most common after several weeks in a cast or boot, particularly in older adults, people with osteoporosis, or anyone whose recovery has involved limited movement for a long time. The ankle can also feel more vulnerable if the fracture was complex or required surgery with plates or screws. Early stiffness and swelling are often triggered by standing or walking for longer periods than the joint is ready for, or by uneven ground during the first few weeks of recovery.Once the cast or boot is removed, the focus shifts from protection to gradually regaining movement and function. Your doctor or surgeon will explain how much weight you can put through the leg and how quickly to build this up. During this period, the ankle often feels vulnerable, especially when you move beyond controlled settings like a hospital corridor or your living room. The first few weeks are about rebuilding confidence as much as strength. Bone healing continues for several months, so gradual loading remains important even after the cast is off.An ankle–foot brace can be particularly helpful at this point. The FootReviver brace supports the ankle in a straighter position and limits how far it can suddenly roll inwards or outwards. This makes early steps, short outdoor walks and uneven surfaces such as small kerbs or gentle slopes feel more secure. It adds an extra layer of protection against the unplanned twists that can be worrying when you are first back on your feet.The brace also provides gentle compression around the ankle and lower leg, which can help manage the swelling that often lingers after a fracture or operation. Swelling tends to increase as you spend more time upright during the day. Containing it can reduce the feeling of heaviness and make it easier to move the joint within the range recommended by your medical team. This can make rehabilitation exercises more comfortable and effective.As strength, movement and confidence improve, the way you use the brace will usually change. At first, you might wear it for most outings and any walking away from home. Later, it might be kept for longer walks, busier days or less even ground, while shorter indoor distances are managed without it. The pace of this change depends on the nature of your injury, how your healing is progressing, and your general health. It’s best agreed with your surgeon or therapist, who can help you balance protection with gradual independence.It’s important not to use a brace instead of following specific instructions about weight‑bearing or walking aids. If your doctor has asked you to keep weight off the leg, to partial‑weight bear, or to use crutches or a stick, those instructions remain in place whether or not you are wearing a brace. The brace is designed to work alongside those measures, not to replace them.If, during this period, you notice a sudden increase in pain, a change in the shape of the ankle or foot, a new feeling of something moving incorrectly inside the joint, or signs such as fever, redness and warmth around the area, contact your medical team promptly. These can indicate problems with healing or infection that need to be checked without delay.Drop foot and walking safetyWhen the front of the foot doesn’t lift properly, walking can quickly become difficult and worrying. Toes may scrape on carpets, catch on small steps or drag on uneven ground. Many people find themselves lifting the knee higher than usual or swinging the leg outwards to clear the foot. Over time, this can feel tiring and awkward, and the fear of tripping can lead to avoiding certain routes or going out less often.This difficulty lifting the front of the foot – known as drop foot – usually happens because the nerves or muscles that pull the toes and foot upwards aren’t working as they should. The cause can occur at different levels. Sometimes it’s due to a nerve being irritated or compressed around the knee or lower leg. In other cases, there may be a broader nerve problem affecting the leg, or a condition involving the brain or spinal cord. In some people, muscle disease is the cause. Whatever the reason, the result is less control over lifting the foot at the right time in the walking cycle.Drop foot can develop gradually, for example after long‑term nerve irritation, or appear suddenly after a stroke or nerve injury. It’s more common in people with diabetes, neurological conditions such as multiple sclerosis, or those recovering from leg or back surgery. The problem often becomes more noticeable when you’re tired or walking on uneven ground, where the foot has to lift and land more precisely.When the foot doesn’t lift reliably, trips and stumbles become more likely. Everyday surfaces such as pavements, doorways and small steps into or out of rooms can all pose a risk. Many people with drop foot become very cautious about where they walk and may limit how far they go to reduce the chance of falling. This can affect independence and confidence, and often leads to reduced fitness and mobility over time.An ankle–foot brace can help by changing how the foot is held and how the ankle moves as you walk. The FootReviver brace supports the foot closer to a right angle with the lower leg, rather than allowing it to hang down. This helps the toes clear the ground more reliably when the leg swings forwards. The brace also supports the ankle as the heel lands and as weight moves forwards over the foot, guiding the joint through a more controlled movement. Many people find that this makes each step feel steadier and reduces the need for exaggerated movements at the knee or hip.The main aim of using a brace in drop foot is to improve walking safety and make movement less tiring. It’s usually worn when you’re up and about, particularly outdoors or in busier areas where a fall would be more serious. Some people continue to use it long term as part of their daily walking, while others may combine it with other aids or treatments depending on how their condition changes over time.The brace doesn’t treat the underlying nerve or muscle problem, but it works alongside other care. This may include physiotherapy, exercises, and in some cases electrical stimulation or surgery, depending on the cause. A doctor, neurologist or rehabilitation specialist can help identify the best combination of treatments for you and advise on exactly when and how to use the brace.If drop foot comes on suddenly, especially if it’s accompanied by other symptoms such as weakness in other parts of the limb, changes in sensation, difficulty speaking or changes in the face, seek urgent medical assessment. These features can indicate a serious underlying problem that needs immediate attention.Ankle muscle and tendon overloadNot every ankle problem begins with a clear twist or fall. Often, discomfort builds gradually after doing more than usual. That might mean walking further or more often, starting a new exercise routine, or beginning a job that involves more time on your feet. The ankle may feel tight, achy or tired rather than sharply painful, and it often feels worse towards the end of the day or after a busy spell.This type of problem is common in people who spend long hours on their feet, start new exercise routines, or return to activity after a break. In these situations, the muscles and tendons around the ankle are exposed to more load than they can comfortably handle. Each step or period of standing places small, repeated forces through these tissues. When that load builds up faster than the tissue can adapt, microscopic strain develops within the fibres. The body responds with local inflammation and sensitivity — what we describe as overload. It doesn’t necessarily mean you’ve caused serious damage; it usually reflects asking tissues to do more than they’re ready for.Everyday habits can add to this overload without you realising. Repeatedly walking or running on sloping or uneven ground places extra demand on the tendons that turn the foot inwards or outwards. Standing for long periods with more weight on one leg than the other, or spending much of the day in footwear that offers little ankle support, can also shift more work onto certain muscles and tendons. Over time, these patterns can create a background ache that flares when you do more. It’s also common for this to happen after returning to activity too quickly following rest or injury, before the tissues have fully adapted again.Managing this type of overload usually involves adjusting activity and building strength. Reducing distances slightly, varying the surfaces you walk on, breaking up long standing periods, and increasing activity gradually rather than suddenly all help the tissues adapt. Strengthening exercises for the muscles around the ankle and lower leg then improve their ability to cope with those demands. Recovery is often steady rather than quick, but consistent progress helps prevent recurrence.An ankle–foot brace can be useful as part of this process, particularly for days or tasks that you know will challenge the ankle more. By supporting the joint in a straighter position and reducing unwanted wobble or twist, the FootReviver brace cuts down the amount of fine corrective work the muscles have to do with every step. Many people find that wearing the brace for longer walks, demanding work shifts or busier days on their feet makes those activities feel less tiring and more manageable.The compression the brace provides can also help if there’s mild swelling or a feeling of fullness around the ankle after activity. A more contained ankle can feel more comfortable and easier to move, which often makes it simpler to stick with the gradual increase in activity and exercises needed for longer‑term improvement.It’s important not to rely on the brace alone without addressing how much you’re asking your ankle to do. If you continue to overload the muscles and tendons without giving them time and support to adapt, symptoms are likely to return whenever the brace is removed. A doctor, physio or podiatrist can help you plan how to combine brace use, activity changes and strengthening so that your ankle becomes more resilient over time.If pain comes on suddenly and severely, if you feel or hear a snap, lose function straight away, or notice rapid swelling and bruising after a specific movement, seek medical assessment promptly. These signs can suggest a more significant tendon or muscle injury that needs specific advice and treatment.Safety and when to seek adviceAcute injury warning signsIf you’ve recently injured your ankle or foot and notice very severe pain, that the joint looks out of place, you can’t put any weight at all through the foot, or swelling comes on very quickly, seek urgent medical assessment before using a brace. These signs can point to a fracture or another serious injury that needs specific care.In the first few days after a significant injury, some pain and swelling are expected, but they should start to ease with rest and appropriate management. If pain stays very high and doesn’t improve, or if swelling and discomfort are clearly getting worse instead of settling, you should be reviewed by a doctor. Using a brace alone in these circumstances can delay important treatment.Circulation, nerve or skin concernsWhile wearing the brace, check the skin and soft tissues underneath regularly. If you see redness that doesn’t fade after removing the brace, blisters, broken skin, or any sign that the skin is being rubbed or damaged, the fit may need adjusting and you should seek advice.Changes in skin colour below the brace — such as the foot becoming unusually pale or blue — or a noticeable change in temperature, numbness or tingling can be warning signs that circulation or nerve function is being affected. If you notice any of these, remove the brace and get medical advice promptly.Nerve‑related or general health concernsIf you suddenly find it difficult to lift your foot, especially if this happens alongside other symptoms such as weakness in the leg, changes in sensation, slurred speech, facial changes or a sudden loss of balance, seek urgent medical assessment. These signs can indicate a serious underlying condition that needs immediate attention.More general health changes such as fever, feeling generally unwell, or spreading redness and warmth around the ankle or foot may point to infection or another health problem. In these situations, contact a healthcare professional without delay.Driving and this braceDriving depends on being able to move your ankle freely, quickly and accurately to control the pedals. This brace is designed to limit ankle movement and hold your foot in a more fixed position, which can affect how quickly and precisely you press and release the pedals.For safety, you shouldn’t drive while wearing this brace. Doing so may slow your reactions and increase the risk of an accident that could harm you or others. When you’re considering driving again after an ankle or foot problem, discuss it with your doctor and follow any legal or licensing guidance. Only resume driving when you can control the pedals safely without the brace and have been advised that it’s appropriate to do so.General advice and next stepsThis information is general and doesn’t replace an in‑person assessment or diagnosis. The brace is one part of supporting and protecting the ankle and foot. Decisions about using it, and about your activity levels while wearing it, should take account of your diagnosis, any other health conditions and any treatments you’re receiving. If you’re unsure, it’s always reasonable to speak with a doctor, physiotherapist or podiatrist who can advise on your particular situation.No brace can guarantee a cure or a specific outcome, but used in the right way it can make movement more manageable and safer while other parts of your treatment are in place. Recovery times differ depending on the type of injury and your general health, so it’s important to follow the plan agreed with your healthcare professional. This brace isn’t designed to prevent or treat blood clots or circulation problems such as deep vein thrombosis (DVT). If you notice swelling, pain, or warmth in the calf that’s new or worsening, seek medical advice promptly. If in doubt, pause and ask.Quick recap: what this brace offersA semi‑rigid ankle–foot brace from FootReviver, made to support and control the ankle and foot rather than completely immobilise them.Designed to support adults with ankle and foot problems such as sprains, strains, post‑fracture recovery, tendon issues, arthritis, drop foot and post‑operative needs.Firm frame with a stable base and aluminium splints along the sides, front and back to help hold the ankle and foot in a straighter position, reducing sudden twisting and rolling that can strain ligaments and joint surfaces.Multiple fully adjustable buckled straps that secure the brace and let you set the level of support and compression to match your activities and stage of recovery.Compression around the ankle and lower leg to help manage swelling, ease the feeling of fullness and tightness, and support healing tissues.Positioning support that assists with toe clearance and more controlled steps in conditions such as drop foot and long‑standing instability.Lightweight, breathable, non‑bulky materials and padding around key bony points for more comfortable wear, with the option to use the brace with suitable footwear once your doctor or therapist advises this is safe.Available in three sizes (Small UK 3–5, Medium UK 5–8, Large UK 8–11) to fit a range of foot sizes.Can be used in the early days after certain soft‑tissue ankle injuries, where a doctor has recommended protection and compression, to help protect and support the area.Comes with a 30‑day money‑back guarantee.This FootReviver design aims to offer more control than a simple elastic sleeve, while being easier to live with day to day than a full rigid boot.Bringing it all together: how this brace helpsThe ankle and foot work hard every day and take on many different stresses. A sudden twist can strain the ligaments on the outside of the ankle. Repeated loading can irritate tendons such as the Achilles or the plantar fascia under the heel. Wear‑and‑tear changes in the joints can cause stiffness and aching. Nerve or muscle problems can alter how the foot lifts and lands, increasing the risk of trips and falls. Any of these can make walking, standing and returning to normal activities feel like a real challenge.The FootReviver Ankle Splint Foot Brace & Post‑Op Cast Support is designed to help in these situations by holding the ankle and foot in a more controlled position, helping to manage swelling, and adding an extra layer of stability when you move. For example, if your ankle tends to roll inwards after a sprain, the brace’s side supports help limit that roll. If your toes catch the ground when you walk, its foot support helps lift the foot enough to clear the surface. By limiting the extremes of twist and bend that often trigger pain, and by holding the foot closer to a right angle to improve control and toe clearance, it can make many everyday tasks feel more secure and manageable when used as part of a wider treatment plan.If the pain, stiffness or instability described here sound familiar, and a doctor, physio or podiatrist has suggested that an ankle–foot brace is appropriate for you, this FootReviver brace is one option to consider. It’s worth discussing it with the person overseeing your care so you can decide together how best to use it alongside exercises, footwear changes and any other treatments, to support both your recovery and your longer‑term ankle and foot health. Used correctly and with professional guidance, it can help you move with greater confidence as your ankle and foot recover.
Ankle Supports