Ankle Brace for Sprains, Strains, Fractures, Achilles Tendonitis & Heel Pain
$11.24
$19.78
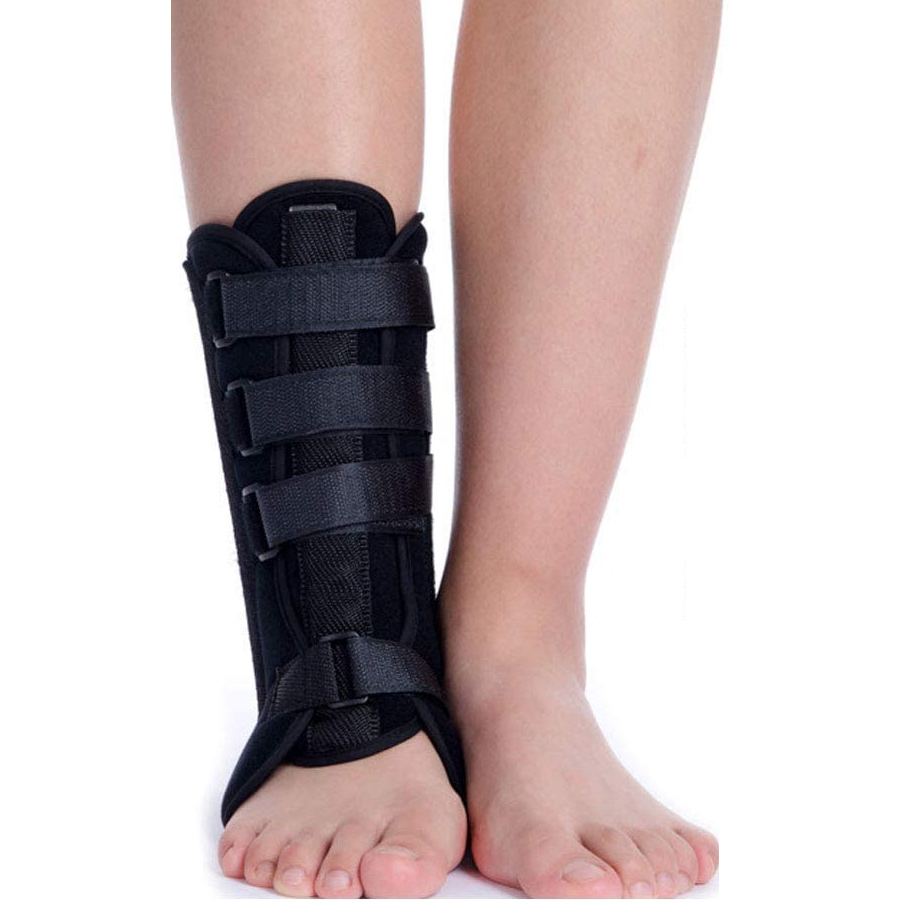
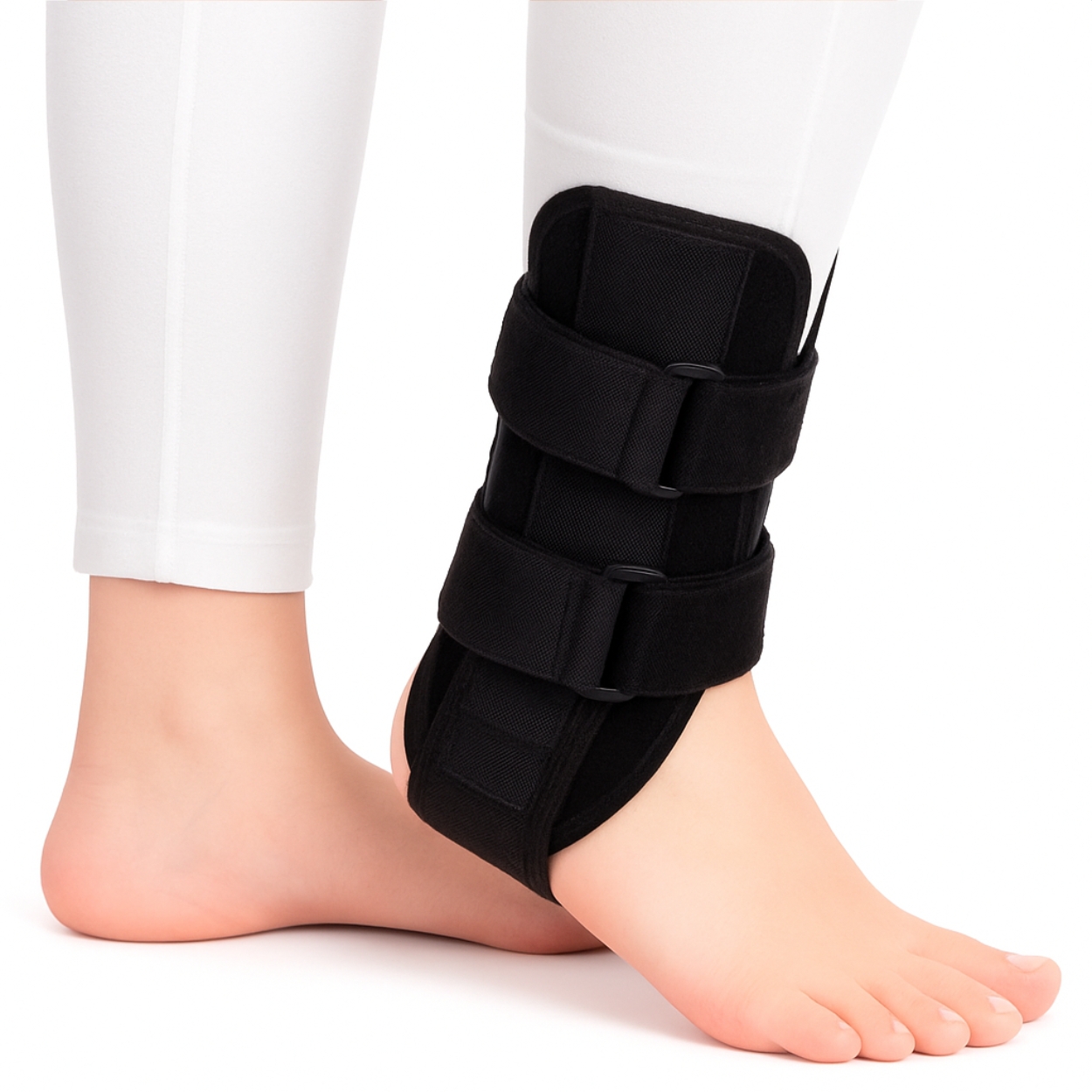
Who this ankle brace is for and what you’re struggling withIf your ankle feels painful, weak or unreliable, everyday activities can slow right down. You may find yourself planning what you do around what your ankle will tolerate. Walking outside, using stairs, standing for parts of the day, or crossing slightly uneven ground can all begin to feel like a risk rather than something you do without thinking.You might notice a sharp catch or pain around the bony bumps on either side of your ankle when it rolls or tips unexpectedly. These are the areas where key supporting ligaments sit. You could feel a dull ache or stiffness at the front of the ankle when your knee moves forwards over your foot, such as when you walk down a slope or go downstairs. This happens because the front of the ankle joint surfaces and capsule are compressed more firmly in that position.Pain, tightness, or a dragging sensation at the back of your heel or just above it when you push off is also common, as this is where the Achilles tendon and its attachment into the heel bone work hardest. For many people this is one of the reasons stairs and hills feel particularly awkward or painful.This brace is designed for adults who recognise some of these problems in their own ankle. You may have recently twisted or rolled your ankle. The swelling and bruising have mostly settled, but it still aches or feels unsteady. In many cases this means your foot suddenly turned inwards (more commonly) or outwards under your body weight, stretching the ligaments on that side that would usually limit that movement.You may have had a more serious injury such as an ankle fracture and are now moving out of a cast or boot into a more active stage of recovery. The bone has healed or been clinically cleared, but the supporting ligaments, muscles and joint capsule have been held still and are weaker and stiffer, so the ankle feels unsure, particularly on stairs, slopes or uneven ground.Your ankle may have given way more than once, and you find yourself scanning the ground for anything that might make it roll again. You might walk more stiffly or keep your steps small and guarded because you do not fully trust that ankle. You may feel a persistent ache or sharp pain around the back of the ankle or just above the heel, especially when you push off, climb stairs, or walk for longer periods. These activities make your ankle bend further over your foot and increase the pulling force through the Achilles tendon and heel structures, which can set off sensitive tissue there.You may also have tried a soft elastic sleeve or light support, but it feels more like a comfort layer than something that truly holds your ankle where you want it. It may warm and compress the area but not really prevent the sharp tilts that worry you.In simple terms, this brace is for people whose ankle needs more than light compression. It is a rigid, side‑splinted brace with a built‑in cushioned heel pad and adjustable elastic straps, designed by FootReviver and supplied by Nuvoahealth. FootReviver developed it specifically for ankles that have moved on from a boot or cast but still feel too loose or vulnerable for a soft sleeve. It is built to give firm guidance to your ankle in the directions where it is most vulnerable, especially the inward and outward rolls of the heel and ankle that cause many sprains and episodes of giving‑way.The brace supports your heel and softens impact under the back of your foot, helping your heel bone, Achilles attachment and natural fat pad to tolerate walking better. At the same time, your toes and the rest of your foot remain free, so your step can still rock forwards in a natural way instead of feeling locked in a rigid block.This brace is intended for adult use during everyday walking and standing, on your return to usual daily tasks after an ankle injury or immobilisation, and for controlled exercise or activity where extra stability around the ankle is needed. That might include predictable, slower movements like planned rehabilitation exercises or steady walking. It is not designed as a substitute for a cast or boot in the earliest stages of a fracture, and it is not intended for swimming or for very high‑impact, collision‑type activities with repeated hard landings or strong, sudden forces that a semi‑rigid brace is not built to absorb. If you cannot put any weight through the ankle after a new injury, or can only manage a few steps with severe pain, you usually need assessment and different support before a brace like this is considered.What is actually happening inside your sore or unstable ankle It is easy to think of your ankle as a simple hinge that should bounce back quickly. In reality, it is a complex joint involving several bones, many ligaments, a network of tendons, and a capsule filled with synovial fluid – the slippery liquid that lubricates movement. When one part is injured or held still, the way the whole joint works can change.Understanding what happens inside your ankle after an injury often helps people realise they are not imagining things when it still feels sore and unreliable weeks or months later.Ligaments after a sprainLigaments are strong bands of connective tissue that connect one bone to another and help keep joints stable. Around your ankle, they sit mainly on the inner and outer sides, running from the leg bones down to the foot bones. They hold the bones of your ankle in their proper relationship, help limit how far the ankle joint can move in each direction, and send information to your nervous system about joint position and movement. This joint position‑sense is called proprioception – your ankle’s ability to tell your brain exactly where it is.Most ankle sprains involve the ligaments on the outer side of the ankle joint. A typical rolled ankle happens when your foot suddenly turns inwards underneath you as your body weight moves over it. Your heel and ankle roll inwards towards the opposite leg and the ligaments on the outer side of the joint are forced beyond their normal range. Less commonly, your foot turns sharply outwards and the ligaments on the inner side are stressed instead.When you sprain an ankle, these ligaments are stretched beyond their usual range. In a mild sprain, the fibres are stretched and a few may be microscopically damaged, but the overall structure is largely intact. In a moderate sprain, more fibres are torn and the ligament becomes longer and weaker. In a severe sprain, the ligament may be completely torn or pulled away from the bone. In all cases, your body responds with inflammation: fluid and repair cells move into the area in and around the ligament and capsule, causing swelling, warmth and stiffness.Over time, new collagen fibres lay down to repair the damage. However, the new tissue may be a little longer than the original, leaving the ligament slightly looser, and the nerve endings in the ligament may not send position signals as effectively for a while. So even when bruising and obvious swelling have reduced, the consequences are often similar across mild, moderate and severe sprains. Your ankle can roll or tip more easily than before, especially when you turn quickly, walk on uneven ground, or are tired and less alert, and you may feel less sure where your foot is without looking.When joint position‑sense is dulled in this way, your brain has less precise information, so your muscles react a little more slowly to correct a wobble, and the joint can feel sloppy or as if it might go again at any moment. Ligaments can improve, but this slower, less precise feedback is one reason the ankle takes longer to feel normal than many people expect.Even a mild sprain can leave your ankle feeling not quite right for several weeks if you go straight back to full activity without support or rehabilitation. If you keep rolling it, even just a little, the ligaments stay irritated and can stretch further. Over time this can increase the likelihood of the joint feeling looser and can increase strain on the cartilage surfaces – the smooth, slightly springy coverings on the bone ends inside the joint – making stiffness and aching more likely.Muscles and tendons after injury or less useMuscles and their tendons around your ankle play a key role in fine control. A tendon is the strong cord that connects a muscle to bone. On the outer side of your ankle, the peroneal muscles and tendons run down from the outside of your lower leg, behind the outer ankle bone, and into the outer side of your foot. They help stop your heel and ankle from rolling too far inwards. On the inner side and front, the tibial muscles and tendons run behind the inner ankle bone and across the front of the ankle to help support your arch and lift the front of your foot. At the back, your calf muscles merge into the Achilles tendon, which attaches onto the back of your heel bone. Together they manage push‑off and help control how you land on your heel.After an injury, or if you naturally move less because of pain, these muscles may weaken and lose endurance surprisingly quickly. Your walking pattern often changes: you may shorten your stride, avoid putting full weight through the injured leg, or turn your foot outwards to feel safer. Some muscles are then overworked while others are underused, leading to imbalances around the ankle joint.For example, turning your foot outwards shifts more work to the outer muscles and tendons. Avoiding full weight on the sore leg makes your other leg, hip and back work harder to keep you moving. A shorter stride means the calf and Achilles tendon on the sore side do less push‑off and gradually lose capacity.Tendons do not cope well with repeatedly doing more than they can comfortably manage at that time. If you ask them to do too much walking, standing, climbing or descending steps, tiny areas of tissue irritation can build up faster than your body repairs them. The tendon thickens and becomes more sensitive, and everyday loads such as walking up a gentle slope, climbing a few stairs, or pushing off to step forward can start to cause a sharp or dragging pain around that specific tendon.These changes usually develop over days and weeks of similar activity rather than from one single incident. A common mix of symptoms is stiffness and soreness in the ankle or tendon area when you first move after rest, especially for the first few steps, some easing as you warm up, then an ache or sharper pain later in the day or the next morning if you have done more than the tendon can currently tolerate. If you continue to overload the tendon without support or a gradual rehabilitation plan, the problem can become longer‑lasting and more stubborn to settle. The tendon is not torn all the way through, but it never quite catches up between bouts of activity, so irritation builds instead of resolving.That is why the first few steps after sitting can feel much sharper than the rest of the walk, even though the tendon sometimes feels a bit easier once you get going.Joint surfaces, capsule and stiffness after being held stillYour ankle joint is enclosed by a capsule – a tough, fibrous envelope that surrounds the joint, helps contain the synovial fluid inside, and contributes to stability. Inside the joint, the ends of the bones are covered in cartilage, a smooth, slightly springy surface that allows the bones to glide over one another with very little friction. Synovial fluid made by the joint lining feeds and lubricates this cartilage and spreads more effectively when the joint moves.If you have had a fracture, or a serious ligament or tendon injury, you may have needed a cast, boot or other immobilising device. This is often necessary to protect healing tissues, but it has consequences for how the joint behaves afterwards. While your ankle is held still, the joint capsule can tighten, the cartilage surfaces do not move through their usual range, and synovial fluid does not circulate as effectively because movement is one of the main ways it is spread across the joint surfaces. When these structures are not moved regularly, they lose some of their easy glide and the joint feels stiff when you first try to bend it.When you start to use your ankle again after weeks in a cast or boot, the joint often feels stiff, weak and unfamiliar. You may struggle to bend your ankle forwards so your knee moves over your toes, or backwards so your toes move up towards your shin. Stepping down from a small step or kerb can be especially difficult because it asks the ankle joint to bend more and take a sudden increase in load. The front of the ankle joint and capsule are compressed more firmly in this position, and if you push too aggressively at first, the capsule and surrounding tissues can become sore and irritated.You may unconsciously avoid moving your ankle through its full range, taking short, guarded steps and placing more stress on other joints such as your knees, hips and lower back. Keeping the ankle stiff means your knee and hip have to bend more to achieve the same stride.Why you have “good days” and “bad days”As you come out of an ankle injury, it is very common to have good days and bad days. On a good day, the joint feels relatively settled, so you walk further, stand longer, or try a few more challenging tasks. The next day, your ankle can feel more swollen, stiff or painful again.This mix of easier days and harder days often reflects the current limits of your healing ligaments, tendons and joint surfaces – in other words, how much walking, standing and twisting your ankle can cope with without flaring symptoms – and the amount and type of weight and movement you have put through it. For example, a 15–20 minute flat walk might be fine one day, but doubling that distance, adding slopes, or spending hours on hard floors may push those tissues beyond what they can manage right now. Balance and control also take time to rebuild, so the joint may still struggle with sudden, multi‑direction movements even if straight‑ahead walking on flat ground feels reasonable.Without the right support and a gradual, structured build‑up of activity – steadily increasing walking and standing in small steps rather than jumping straight back to previous levels – it is easy to fall into a cycle of doing more on good days and then paying for it afterwards. Your ankle feels a bit better, so you do more. A small twist, a longer day, or an unexpected step overloads it again. Pain and swelling increase, so you move less and protect it. Muscles and ligaments then lose a bit more strength and responsiveness. The next time you challenge it, it copes even less well.Many people say they feel back to how they were weeks earlier after one demanding day – for example, you might comfortably manage a 20‑minute walk one day, then feel as stiff and sore as you did much earlier in your recovery after twice that distance or a full day on hard floors. Knowing that this often comes down to how much healing tissues have been asked to do, rather than just “being unfit”, can be reassuring.A well‑designed brace aims to help break that cycle by guiding your ankle within a safer range, helping to reduce the number of sharp twists and painful lapses in confidence, and making it easier to rebuild movement and trust progressively. Over time, a useful sign of progress is fewer extreme swings between good and bad days, even if some ups and downs remain.How this rigid ankle brace helps at that stage of recoveryOnce you understand what happens to ligaments, muscles, tendons and joint surfaces after an injury or a spell in a cast or boot, it becomes clearer why an external support around your ankle is sometimes needed.If ligaments are slightly lax and slower to signal position, you are more dependent on muscles and tendons to control each step. In sudden or awkward movements, they may not react fast enough to prevent another roll, especially when you are tired, on uneven ground, or distracted. This shows up as sudden giving‑way of the ankle, a sharp twinge on a mis‑step, or a constant feeling that your ankle is close to its tipping point.If muscles and tendons around the ankle are tired or irritated, they cannot provide a firm, steady base throughout the day. The ankle can wobble more as you stand or walk, which in turn irritates the ligaments and joint surfaces again. Normal muscle tiredness feels like heaviness that settles with rest. Irritated tendons and muscles give more localised pain that persists or worsens after activity.If your ankle joint has been stiff from immobilisation, you may not yet move smoothly through the full range it needs for normal walking, stairs and slopes. Any unexpected twist or uneven surface can feel much more threatening because the joint has less room and time to give before painful structures are stressed. You may find yourself keeping the ankle stiff and over‑using your knee and hip to compensate.This FootReviver brace wraps a rigid external structure around your ankle with semi‑flexible fabric where movement is still useful. The aluminium side splints sit in padded panels on either side of the ankle and extend a couple of inches above the joint. Because of that extra height, when your heel and ankle start to roll inwards or outwards, the splints can resist that roll earlier, rather than waiting until you are close to the end of the movement.By limiting how far and how quickly the ankle can tip inwards or outwards, the brace reduces the likelihood of the sudden rolls that overstretch ligaments. It gives your ankle a more predictable path for movement, so each step feels less wobbly and more controlled. You can also adjust it to match how much support you need on a given day – for example, a firmer setting on days with more walking, uneven ground or end‑of‑day fatigue, and a slightly gentler setting on days when you are on your feet less.At the same time, the open front around the ankle and the absence of a rigid shell over the foot mean your ankle can still bend forwards and backwards so you can walk, sit down and stand up, and go up and down stairs. That is important for recovery: you want to protect against the risky sideways tilt without freezing the joint in one position.The brace does not replace the need for strengthening, balance training and a gradual, step‑by‑step return to activity. Those are still essential if you want your own muscles and ligaments to resume more of the stabilising work over time. The brace is there to cut down painful slips, jolts and minor re‑sprains that keep setting you back while you rebuild strength and control.How this rigid brace differs from softer sleeves and wrapsLighter elastic sleeves and simple wraps can be useful when ankle pain is mild, settles quickly after short periods on your feet, does not cause giving‑way, and is not stopping you from walking normally. They can be a reasonable choice if there is no history of repeated giving‑way and you mainly want a little warmth and gentle compression around the ankle.However, because they are stretchy in all directions, they usually move with your ankle rather than placing clear limits on risky movements. When your heel and ankle suddenly try to roll inwards or outwards, a soft sleeve does not offer much resistance, so your ligaments and tendons still absorb most of that force. In that situation, a light sleeve often feels more like a comfort layer than a firm support when you are nervous about re‑spraining.This FootReviver brace with its fixed aluminium side splints responds differently when your ankle starts to roll. The splints are built into the side panels rather than being removable inserts, so they do not shift or twist inside pockets. They give a firmer stop in the inward and outward directions while still allowing useful bending forwards and backwards. Because each splint runs up above the ankle joint, when the ankle starts to tip, the brace can push back with more leverage, resisting that movement earlier in the roll.Two separate elastic straps sit over the top. One lies close to the ankle joint and one slightly higher on the lower leg. This lets you set more support near the joint where you feel least secure, and a little less higher up if that feels more comfortable – something a single central strap cannot do as precisely. Compared with many basic braces that use shorter plastic stays and one strap, this longer aluminium splint and twin‑strap design give earlier resistance to rolling and a more tailored fit around the ankle.In everyday practice, most people move through stages of support. In the earliest stages of a severe injury or fracture, a cast, boot or similar device may be needed to restrict movement almost entirely. As healing progresses and weight‑bearing begins, a rigid or semi‑rigid brace like this is often used to support the ankle while allowing functional movement. Later, as strength and control improve, people often move on to lighter soft sleeves, simple wraps or taping, and eventually to no external support.Within that progression, this brace usually sits in the middle and later stages: when you are ready to move more but still need a strong, reassuring frame around your ankle. As your own muscles, ligaments and balance responses improve, a clinician can help you decide when to use the brace mainly for longer days, uneven ground or more demanding activities, and when it is reasonable to rely more on your own control.How this brace is built – and why those design choices matterStructural design, coverage, and open ankleThe brace is built around two supportive side panels. One runs along the inner side of your ankle and lower foot, beside the bony bump on the inside. The other runs along the outer side in the same way. Each panel contains a rigid aluminium splint that extends a couple of inches above your ankle joint. Because the splints reach higher than the joint itself, they have more leverage over tipping forces. When your heel and ankle try to roll inwards or outwards, the long splint acts like a lever arm, pushing back along its length and limiting how far and how quickly the joint can tilt.Under your heel, a cushioned pad links the two side panels. This pad is part of the brace, not a loose insert, so it stays aligned with the splints as you move. It supports the back of your foot and heel bone and spreads pressure more evenly under this area, reducing sharp, localised impact on sensitive tissues such as the heel bone, the attachment of the Achilles tendon and the natural fat pad. By slightly changing the angle between your heel and lower leg, it works like a small heel lift: your heel sits a little higher than it would otherwise, so the Achilles tendon and heel structures are not stretched to their full length on each step. This reduces some of the bend required at your ankle and lessens the stretch and strain through the Achilles tendon and heel area.The front and back of your ankle remain open. There is no rigid panel across the front of your shin or over the top of your foot, and no hard shell behind the Achilles tendon. This means your ankle can still bend forwards and backwards within a controlled range, which is essential for walking, sitting down into a chair, and rising from it. Your toes and the rest of your foot remain free, so the natural rocking motion of the foot from heel to toe can still take place. Your forefoot can feel the ground more normally, giving your nervous system useful feedback for balance and making the brace easier to accommodate inside footwear than a full shell that covers the whole foot.The fabric connecting these parts of the brace is a padded, semi‑elastic synthetic material. It is firm enough to hold the splints and heel pad against your skin so that they move with you rather than sliding around, but it has enough give to allow small, comfortable adjustments as you move, instead of feeling like a hard, unforgiving shell. Padding is concentrated around the ankle bones and heel, where people most often report rubbing with other designs, and seams are placed away from these points to help reduce irritation.The splints are fixed in place as part of the brace’s structure. This avoids the common problem of removable stays shifting in use or being refitted unevenly, and means you get a consistent level of side‑to‑side control each time you put the brace on. If you and your clinician decide you are ready for a softer or lighter support, the usual next step is to move to a different type of brace or sleeve rather than altering this one.Adjustable straps, fit, and compressionAcross the top of the brace sit two separate elastic straps, each with its own buckle. The lower strap sits closer to your ankle joint; the upper strap sits slightly higher on your lower leg. Each strap wraps fully around your ankle and foot, passes through its buckle and folds back on itself. You pull it to the tension you want and then secure it.Because there are two straps, you can set more support where your ankle feels most vulnerable. For example, you might choose a firmer setting on the lower strap, close to the ankle joint, and a slightly gentler setting on the upper strap. You can also change the tension from day to day – for instance, using a firmer setting when you expect more walking or uneven ground, and easing it a little when your ankle feels more swollen.Because the straps are elastic, they provide gentle, even pressure around the ankle. This can give a reassuring, contained feeling and may assist the normal movement of fluid in and out of the area when you are active. The aim is snug but not strangling: the brace should feel firm and secure, as though it is giving your ankle a reliable frame, but it should not cause pins and needles, numbness, marked skin indentation, or significant colour changes in your foot or toes. If it does, the straps are likely too tight and should be eased.Support mechanics: how it changes movement and loadThe side panels, splints, heel pad and straps combine to change the way forces are handled by your ankle with each step.When you place your foot down and weight begins to load through the ankle joint, the brace helps guide the ankle into a more central position rather than letting it drift towards an inwards or outwards lean. This reduces repeated stretching of the inner and outer ligaments described earlier. If your heel and ankle start to tip inwards or outwards, the splints resist this motion before the ligaments are stretched to their painful limit.The heel pad provides a cushioned platform, softening the shock that travels up through your heel, ankle and leg at heel contact and moderating sudden changes in angle during the middle part of the step. By lifting the heel slightly and evening out pressure, it also reduces the peak pulling force through the Achilles tendon and the back of the heel when you push off.For recurrent sprains and instability, the brace acts as an external check on the movements that caused the original injury. Instead of your ankle ligaments having to absorb the full force of a sudden roll, the splints and side panels take some of that load and limit how far the joint can go. The firm, consistent contact of the brace around your ankle also helps your body sense where the joint is in space, which can support quicker muscle responses. This reduces strain on healing fibres and the risk of another sharp injury from an unexpected mis‑step.After a period in a cast or boot, the brace provides a secure, predictable framework as you start to bear weight and walk more. It makes your steps more consistent, reducing the number of unexpected wobbles that can make you feel unsafe and cause you to tense up. This can make it easier to focus on regaining a more natural walking pattern and on doing rehabilitation exercises, without constantly worrying that the ankle might collapse.For Achilles and heel problems, the heel pad supports the back of your foot and slightly reduces the amount of ankle bend needed at each step, especially at the moment when your heel lifts and your body weight moves forwards. This decreases the stretch and pulling forces at the most irritated part of the tendon or heel area. By keeping your ankle from rolling excessively inwards or outwards, the brace also reduces sideways twisting through the tendon, which can be particularly aggravating. Overall, the brace is designed to make each step feel more even, with fewer sudden jumps in force through sensitive tissues.Making it comfortable enough that you can actually wear itSupport only helps if you can tolerate wearing it. Discomfort is one of the main reasons people stop using braces, so this one is designed with longer wear in mind.The interior is softly padded to cushion the ankle bones and the heel. The fabric is breathable and draws moisture away from your skin, helping to keep the area drier and reducing the chance of chafing and irritation. The inner surface grips the skin or sock slightly so that, once positioned, the brace is less likely to twist or ride up as you move. All edges are smooth and rounded, and seams are directed away from key contact points.Because the main bulk is along the sides of your ankle rather than across the whole foot, the brace can often be worn with slightly roomier everyday footwear, particularly shoes with adjustable fastenings rather than very tight slip‑on styles. It can also be used on its own at home when you are walking around without shoes.Being able to keep the brace on through the times of day when your ankle usually works hardest – such as periods of prolonged standing, longer walks, repeated use of stairs, or moving on uneven surfaces – is what allows the support to help in your recovery. You do not usually need to wear it every waking hour. It matters more that you have it on when your ankle is under most strain.How and when to wear the brace in daily lifeChoosing the right sizeThe brace is available in three sizes, based on approximate UK shoe size:Small: UK 3–5Medium: UK 5–8Large: UK 8–11It is suitable for both men and women and can be worn on either ankle. If one foot is larger than the other, it is usually best to choose the size that fits the larger foot and ankle, then fine‑tune the fit with the straps.When deciding which size to choose, consider your usual shoe size, whether your ankle is currently swollen, and whether you plan to wear the brace over a thin sock or directly against your skin. A thin sock can reduce rubbing and help with hygiene, but it does add a little extra bulk inside footwear. If you are between sizes and have a broader foot or a visibly larger ankle circumference – for example, if swelling is still present – the larger size will often be more comfortable. You can then tighten the straps to achieve the level of support you need. If you have fragile skin or reduced sensation, wearing a thin sock under the brace and checking the skin regularly is particularly important, because you may not feel early rubbing or pressure as clearly.Putting it on and adjusting itThe first few uses are about learning a simple routine and finding strap tension that feels both secure and comfortable.A typical sequence is to sit with your leg supported and place your heel onto the cushioned pad so that the back of your foot rests comfortably on it. Make sure any sock is smooth and there are no wrinkles under your heel. Check that the side panels lie flat along the inner and outer sides of your ankle, with the top edges a short distance above the bony bumps on each side.Bring the lower strap across the front of your ankle, feed it through its buckle, then pull it back on itself to your chosen tension and secure it. Repeat with the upper strap, again pulling to a firm but comfortable tension before securing it.Once both straps are fastened, stand up slowly and take a few careful steps on a flat surface. Notice how supported your ankle feels and whether there are any points of excessive pressure or rubbing. After a short walk – for example, a minute or two around the room – sit down again and re‑check the straps and position. Fabric and padding can settle with movement, so it is often worth making small adjustments at this stage.If anything feels too tight or pinching, if your toes feel numb or tingly, or look unusually pale or dark, or if you notice areas of redness or soreness under the edges, gently ease the straps and test again. The aim is a snug but not strangling feel: the brace should feel as though it is reliably holding your ankle, without causing discomfort further down the foot.As you become familiar with the brace, putting it on becomes quicker and more intuitive. Many people find that spending a little extra time at the start to get the fit right pays off in comfort and support later.Building up wear‑time and choosing when to use itMost people benefit from building up usage gradually rather than wearing the brace all day from the outset. This allows your skin to adapt to the contact and compression, your ankle and lower leg to get used to the changed support, and you to judge how your symptoms respond.A simple approach is to start with shorter periods at home in the early days, such as 30–60 minutes at a time, while you are moving around rather than sitting completely still. If this feels comfortable and your ankle is no more sore or swollen afterwards, you can gradually extend to a few hours at a time. Focus on wearing the brace during periods when your ankle normally feels most vulnerable – for example, when you expect to be standing for a while, walking further than usual, using stairs repeatedly, or moving over less predictable surfaces.These timings are examples rather than rigid rules. Some people will need shorter or longer bouts depending on their condition and background health. Pain that spikes, increased swelling around your ankle, pins and needles, or unusual skin discomfort are signs to ease off and discuss with a clinician if you are unsure. Over the course of days to weeks, with guidance from a clinician where needed, you can adjust how many hours per day you use the brace based on how your symptoms and confidence respond.The brace is intended for everyday walking and standing at home or out and about, and for moving around during the working day if your role involves significant time on your feet or frequent turning and changing direction. In jobs that involve a lot of walking, lifting or twisting on your feet, it is worth checking with a clinician whether this type of rigid brace is sufficient. The brace can also be used for controlled exercise, such as gentle conditioning work, supervised rehabilitation exercises, or exercise sessions where you gradually test what your ankle can do.It is not designed for use in water, for very high‑impact activities with repeated hard landings such as repeated jumping drills or sprint‑type training, or for situations where strong forces from collisions or rapid, extreme movements are expected. Most people only wear this brace when they are up and about and do not need to wear it overnight. If a healthcare professional advises you to wear a support overnight – for example, in certain more complex situations – they should guide you on whether this particular brace is appropriate and how to use it safely.As your ankle improves, you can discuss with your clinician how to move on to lighter supports. For example, you may use this brace mainly for longer outings or uneven ground, or in higher‑demand situations such as recreational sport or busy, crowded environments, and rely on softer supports or no brace for lower‑risk, shorter activities. Strength and balance training remain important as you do this.Care, cleaning, and how long it stays effectiveCleaningLooking after the brace helps it stay supportive and comfortable against your skin. To clean it, hand‑wash the fabric in cool or lukewarm water with a mild detergent. Rinse thoroughly to remove any soap residue, which can irritate the skin. Gently press out excess water without twisting or wringing the material, then leave the brace to air‑dry naturally away from direct heat sources such as radiators or strong sunlight.Avoid harsh chemicals or bleach, which can damage the fabric and irritate your skin, and avoid tumble‑drying or placing the brace on very hot surfaces, which can warp components and reduce support.How long it stays effectiveWith regular, everyday use and good care, the brace is expected to maintain its supportive feel for many weeks to months. How long it remains at its best will depend on how frequently and how intensely it is used, and how tightly the straps are routinely pulled. Wearing it all day during very physically demanding work will wear it faster than occasional, lighter use.Over time, it is normal for the straps to lose some elasticity and grip if they are frequently pulled very tight, for the fabric to show signs of wear at high‑friction areas such as around the heel or strap edges, and for the splints to show minor surface marks from use. You should consider replacing the brace if the straps no longer hold it firmly even when you pull them to a sensible tension, if the splints become noticeably bent or twisted and do not sit straight along the sides of your ankle, or if the brace feels significantly less supportive and your ankle wobbles more than it did when the brace was new.Wearing a brace that has lost much of its structure can give you a misleading sense of security. You may feel as though the ankle is supported, but it may be able to roll further and faster than you realise, reducing the protective effect you are expecting. A simple way to keep on top of this is to check – for example once a month – how easily the straps stretch, whether the splints look straight, and how secure your ankle feels when you first put the brace on. If you are unsure, discuss it at your next appointment with a clinician, who can help you decide whether it is time to replace it.Safety, circulation, and when to seek professional adviceAn ankle brace is one part of managing an injury or longer‑term condition. It does not replace a proper assessment, diagnosis, or treatment plan, and it is not suitable for everyone.This brace does not treat or prevent blood clots, does not take the place of a cast, boot or other immobilisation device when those are required, and is not a substitute for medical review after a significant new injury. Blood clots are clumps of blood that can form in veins, particularly in the legs, when movement is reduced for a period. Being injured and much less active for long stretches can be one contributing factor. The main risk is prolonged immobility rather than the brace itself compressing the leg.If you notice symptoms such as unexplained swelling, warmth, or pain higher up in your leg, or any sudden, unexplained shortness of breath or chest discomfort, you should seek urgent medical advice straight away.When to get advice before using the braceYou should consult a GP, physiotherapist, podiatrist or another appropriate clinician before using this brace if you:have known circulation problems in your legshave recently had surgery to your foot, ankle or lower leghave very fragile or easily damaged skinhave conditions that affect your sensation (for example, you cannot reliably feel rubbing or pressure)have complex medical conditions such as serious heart or vascular disease or illnesses that significantly affect healing and are unsure whether a rigid brace is suitable for you.A clinician can help ensure that the brace is appropriate for your specific diagnosis, that the fit and wear‑time are adapted to your circulation, skin and general health, and that you understand how to use the brace alongside exercises and activity pacing – balancing activity and rest so you do not repeatedly trigger short spikes in pain and stiffness after activity.When to seek prompt professional adviceYou should seek prompt professional advice if:you cannot put weight through the ankle at all after an injury, or you can only manage a few steps with severe painpain, swelling, or a feeling of instability are getting worse rather than gradually easing over days and weeks despite using the braceyou notice obvious changes in the shape of the joint, or episodes where the ankle briefly catches or feels stuckthere is no meaningful improvement over several weeks in a new or recently worsened problem, even though you are using the brace, pacing your activity and following basic self‑care advice.These signs may mean that additional structures are involved, that your current level of activity or type of support is not well matched to your ankle’s needs, or that you would benefit from a more tailored rehabilitation plan. A clinician can confirm what is most likely driving your symptoms, advise on how best to use the brace alongside specific exercises and other treatments, and help you plan how and when to reduce support safely as you improve.How this brace fits common ankle and heel problemsThe same mechanical principles – controlling extreme movements, providing a stable base, and cushioning impact – apply across many ankle and heel conditions. Below are some of the more common situations where this type of FootReviver rigid brace is often used as part of a wider management plan. The anatomy and mechanics sections above explain the general background; these overviews show how they play out in particular problems and how this brace can fit alongside the rest of your treatment.Key ankle and Achilles problemsAnkle sprainsWhen this usually shows up for you After an ankle sprain, there is usually an early phase and a later phase.In the first days and weeks, your ankle is often swollen, bruised and quite painful. Putting weight on that leg can be difficult and you may limp or need crutches. As things settle, you can usually walk more easily on flat ground, but certain moments – stepping off a kerb, turning quickly, or walking on uneven ground – still feel risky. You may feel a sharp jab around the outer or inner ankle if it rolls a little, even if it does not fully give way.You might find that you are comfortable on flat, predictable ground for short distances, but feel anxious or unsteady on grass, gravel, slopes or in crowded places where you cannot watch every step. A brief lapse in concentration can be enough for the ankle to catch or roll again.What is happening in the ankle A typical sprain stretches or tears some of the outer ankle ligaments. Even when these fibres have healed, they can remain a little looser and slower to signal position than before, and in the first few weeks they are also more sensitive and easily irritated.That combination means your heel and ankle tip inwards more easily if you land awkwardly or turn quickly, your muscles have to work harder and faster to bring the ankle back into a safer position, and small partial rolls – not just full sprains – can repeatedly stir up soreness and swelling. Many people naturally shorten their stride, turn the foot out slightly, or keep the ankle quite stiff to feel safer.How this brace can help here In the early and middle stages after a sprain, this FootReviver brace aims to cut down the number of sharp tweaks that keep the ligaments irritated.The rigid side panels and fixed aluminium splints provide a firm barrier against the inward and outward tipping that caused the injury in the first place. Because they extend above the ankle joint, they can resist these movements before the healing ligaments reach their painful limit. The built‑in cushioned heel pad softens impact when you first put weight on the foot, which can otherwise be uncomfortable in recently injured tissues.The adjustable straps wrap your ankle in a consistent, snug way, giving a contained feeling that can make it easier to place the foot down fully rather than hovering on the outer or inner edge. Used during walking, standing and early rehabilitation exercises, the brace helps you reduce the number of minor rolls that keep setting you back, take more normal‑length steps on flat ground with better confidence, and focus on your strength and balance exercises, knowing there is a firm frame reducing sudden twists into painful positions.If you still cannot tolerate putting weight through the ankle at all, or pain is severe, you should be assessed before relying on a brace like this. Once your clinician has confirmed that a rigid support is appropriate, many people find this design helps them feel safer on flat ground and less anxious about small mis‑steps.Ankle instabilityWhen this usually shows up for you With longer‑term ankle instability, the main feeling is often that the ankle is never fully trustworthy, even long after the original sprain.Your ankle may feel as if it could give way at any moment, even on relatively flat ground. Small irregularities in the surface – a loose paving stone, a patch of grass, a ridge in a floor – can trigger sudden wobbles or near‑sprains. Symptoms often feel worse when you are tired, towards the end of the day, or after you have been on your feet a lot.You might avoid surfaces such as grass, gravel or cobbles, walk more stiffly and look down a lot to watch where you are placing your foot, and feel anxious about crowded situations where you might be bumped or have to change direction quickly.What is happening in the ankle Over time, repeated sprains or one significant injury can leave the supporting ligaments and capsule a little stretched and less able to hold the ankle bones firmly together. Joint position‑sense from those tissues can also be less sharp. The result is a joint that rests closer to its tipping point and needs less of a nudge to roll.Your muscles and tendons work harder in the background to try to keep the joint centred, constantly making small corrections. This can be tiring, especially late in the day or on uneven ground. To protect yourself, you may have adopted long‑standing habits such as very small steps, turning the foot outwards, or keeping the ankle quite rigid, which reduce sudden movement but also restrict how freely and efficiently you walk. How this brace can help here In established instability, the brace’s job is to act as a strong, reliable outer frame for a joint that has become too loose to trust on its own in certain situations.The rigid side panels and aluminium splints reduce how far and how quickly your heel and ankle can tip into the inward or outward positions that tend to set it off. The snug, adjustable straps give a clear sense of the ankle being held, which can also improve your awareness of where the joint is in space. The cushioned heel and open ankle area allow you to practise a more natural heel‑to‑toe roll while still feeling that the sides are protected.Used for walking, standing and higher‑demand tasks such as uneven ground or busy environments, the brace aims to lower the chance of sharp, unexpected collapses that further stretch already lax tissues. Many people find that, when they combine this brace with strengthening and balance work, they can gradually extend their walking distance and use more varied surfaces without the same level of anxiety about giving‑way.Post‑fracture and post‑immobilisation supportWhen this usually shows up for you Once a cast, boot, or other rigid support is removed after a fracture or major ligament or tendon injury, it is common for the ankle to feel stiff, weak and unfamiliar. Short indoor walks may feel manageable, but longer distances, outdoor surfaces or slopes can bring on aching and fatigue. Stepping down from a step or kerb, or walking downstairs, often feels particularly difficult or threatening.You may find that you take very small steps on the affected side, avoid putting full weight through that leg, and feel that even small wobbles are alarming, even though the bone itself has healed or been cleared by your clinician.What is happening in the ankle While the bone was healing and your ankle was held still, the joint capsule and surrounding soft tissues tightened, the cartilage surfaces and joint lining did not move through their usual range, and the muscles that normally control and support the ankle became smaller and weaker due to disuse. Balance reactions and confidence in that leg had little practice.When you start using the ankle again, the joint may not bend forwards towards your toes or backwards towards your body as easily. The muscles cannot yet control and steady the joint through the whole movement. Other joints – particularly the knee, hip and lower back – may take more of the strain as you change the way you walk to protect the ankle.How this brace can help here Once your fracture has healed or your clinician has confirmed that the bone is stable, the brace can act as a step between a cast or boot and no external support.The side splints and panels give a firm framework that limits sudden sideways movements and reduces the likelihood of alarming wobbles. The heel pad cushions impact as you reintroduce weight‑bearing, making each step feel less jarring. The open front around the ankle and the lack of a rigid shell over the foot allow you to practise bending the ankle forwards and backwards in a more natural way, within a safer, supported range.In day‑to‑day terms, many people find that this makes first outdoor walks, kerbs and stairs feel less daunting. You can put more even weight through the affected leg with greater confidence, take more normal‑sized steps rather than very short, guarded ones, and focus on regaining smooth movement and strength, rather than constantly worrying that the ankle might collapse.Achilles tendon problemsWhen this usually shows up for you With Achilles tendon issues, typical features include stiffness and pain at the back of your ankle or heel when you first stand up in the morning or after sitting for a while, pain that eases a little once you have taken a few steps then builds again with longer or faster walking, a sharp or dragging pain when you push off more firmly such as going up stairs, walking uphill or speeding up, and a deep ache along the tendon or near its attachment into the heel after prolonged standing or walking.You may find that you avoid pushing strongly off that foot, favour the other leg when stepping up or climbing stairs, and that your usual walks or activities leave the back of the ankle more sore than they used to. These symptoms usually reflect how much strain the tendon built up over the previous day or days, rather than something that changes instantly overnight.What is happening in the tendon The Achilles tendon is a strong band that connects your calf muscles to your heel bone. It has to absorb force when you land on your foot and transmit power when you push off to walk, climb or run. When the tendon is repeatedly asked to do more than it can comfortably handle at that time – for example by a sudden increase in walking distance, hills, speed or standing time after a period of being less active – small areas within the tendon can become irritated and disorganised. The tendon may thicken and become more sensitive to stretch and to sudden increases in force.A typical mix of symptoms is stiffness and soreness when you first move after rest for the first few steps, some easing as you warm up, then aching again if you overdo it.How this brace can help here The brace does not repair the tendon directly, but it changes the way forces pass through your ankle and heel in line with this pattern.The cushioned heel pad can slightly reduce how far your ankle has to bend and how sharply the heel is loaded when you step, especially at the moment your heel lifts and your body weight moves forwards. This can lessen the stretch and pulling force on the most irritated part of the tendon or its attachment into the heel bone. The rigid side panels limit excessive inwards and outwards rolling, reducing twisting forces through the tendon with each step.This often means that walking on level ground, using stairs and managing gentle slopes become more tolerable, with fewer sharp jabs at the back of the heel. The key changes in the tendon still come from a structured exercise programme that gradually increases the load through it. The brace is there to reduce sudden jumps in force through the tendon while you work through that plan. A simple pacing example is splitting a longer walk into two shorter walks with a rest between, rather than doing it all in one go.Other ankle and heel conditions where this brace may be usedAnkle osteoarthritisWhen this usually shows up for you With osteoarthritis in the ankle, people often describe stiffness and a rusty feeling when first moving after rest, especially first thing in the morning or after sitting for a while, and a dull ache that builds with longer periods of walking or standing, particularly on hard surfaces. There may be occasional clicking, grinding, or a sense that the ankle is not moving as smoothly as it once did, and difficulty with slopes and stairs, which require more ankle bend and control.You may find that gentle movement eases stiffness at first but, if you overdo it, the joint becomes more painful and sometimes swells by the end of the day.What is happening in the joint Over time, and sometimes following previous injuries such as sprains or fractures, the smooth cartilage covering the joint surfaces gradually wears down. Some areas may become thinner or rougher, and the space between the bones may narrow in places. The joint can become slightly less stable or well aligned.This means that load is no longer spread as evenly across the joint surfaces. Certain parts of the ankle joint take more pressure, especially during activities that demand more bend or control. Small movements or wobbles can create sharp, localised pressure on already sensitive areas, leading to pain and a feeling of grinding.How this brace can help here The brace can help you manage symptoms by influencing how the ankle moves and how forces are transmitted.The side splints and panels help guide the joint through a more central, controlled path with each step, rather than allowing excessive side‑to‑side wobble. This can reduce sharp, uneven pressures on worn areas of cartilage. The cushioned heel pad softens impact when your foot hits the ground, reducing some of the shock travelling through the ankle.It will not reverse the underlying joint wear, but it can make walking and standing feel more steady and less painful. Many people find they can stand for routine tasks or manage a short local walk with less aching by the end of the day when they use this brace alongside appropriate footwear and pacing.Rheumatoid arthritis in the ankleWhen this usually shows up for you When inflammatory arthritis affects the ankle, people often experience swelling, warmth and stiffness, often worse in the mornings or after rest, with episodes where the joint is much more painful and swollen and less active phases in between. There may be a feeling that the ankle is less stable or less able to cope with uneven ground when it is particularly inflamed.You may feel that the ankle is puffy and tight, that simple walking around the house is uncomfortable on flare days, and that you avoid longer walks or slopes when the joint is especially active.What is happening in the joint In this type of arthritis, the lining of the joint (synovium) becomes inflamed. Extra fluid and inflammatory substances build up inside the capsule, and over time this can affect cartilage, bone and surrounding support structures. This can lead to increased pressure inside the joint, making weight‑bearing painful, a sense of fullness and reduced room for movement, and some weakening or stretching of supporting tissues if inflammation has been present for a long time.How this brace can help here The brace can provide supportive help alongside medical treatment and exercise.The external frame gives extra stability around your ankle at times when inflamed tissues feel less reliable. Gentle, adjustable compression from the straps can provide a more contained feeling and may help with the feeling of fullness and tightness by supporting natural fluid movement. The cushioned heel pad reduces impact on an already sensitive joint.It is important that brace use in inflammatory arthritis sits within a broader care plan, including medication and exercises advised by your rheumatology specialist or other clinicians involved in your care. The brace is not a treatment on its own, but can make standing and walking more manageable during more symptomatic phases, and you may adjust how often you use it between flare‑ups and less active phases, in line with advice from your clinicians.Heel bursitis and heel spursWhen this usually shows up for you Problems around the back or underside of the heel may hurt when you first stand up, especially after rest, and flare after long periods on your feet, particularly on hard floors. They may be aggravated by shoes that dig into the back of the heel or have very hard soles, and can make you change how you place your heel to avoid a specific sore spot.You might be able to point with a fingertip to the painful area: just above the back of the heel where the Achilles tendon meets the heel bone, or directly under the bottom of the heel, slightly towards the inner or outer side.What is happening in the heel With heel bursitis, a small fluid‑filled sac near the back of the heel or near the Achilles insertion becomes inflamed, often from repeated friction or pressure. With heel spurs and related irritation, a bony prominence or the soft tissue attachment under the heel can be irritated by repeated impact or pulling forces. Each step on a hard surface can send a sharp jolt into the already sensitive area.How this brace can help here The brace can support the heel area by providing a cushioned platform under the back of your foot to spread pressure over a broader area, rather than concentrating it on one painful point. It helps keep the heel more centrally aligned, so you are less likely to repeatedly land on just the inner or outer edge to avoid discomfort, and it reduces sudden sideways shifts at the ankle that might increase friction or stress around the irritated structures.In practice, this often means that standing for routine tasks or walking on hard indoor surfaces becomes less sharply painful under or behind the heel. Any footwear or in‑shoe changes your clinician has advised will usually work better on top of this more evenly supported heel.Peroneal, posterior tibial and anterior tibial tendon problemsWhen this usually shows up for you Tendon problems around the ankle and lower leg tend to show up in different, quite specific places.Peroneal tendons, on the outer ankle, run behind the outer ankle bone and into the outer border of the foot. Pain or tenderness just behind and below the bony bump on the outside of the ankle is common, often worse when you walk on slightly uneven ground, sloping paths, or when you push off to the side.The posterior tibial tendon runs behind the inner ankle bone and into the inner side of the foot. Pain or aching just behind and below the bony bump on the inside of the ankle, sometimes spreading into the arch, can build with long periods of standing or walking, especially if your feet roll inwards.The anterior tibial tendon runs down the front of the shin to the top of the foot. Pain or tightness along the front of the lower leg down towards the top of the foot tends to flare when you lift your toes repeatedly, walk downhill, or do a lot of stepping up and down. In all of these, pain usually builds gradually with repeated use rather than from a single incident.What is happening in these tendons These tendons help control how your foot rolls in or out, support the arch, and lift and place the front of the foot when you walk. When they are repeatedly asked to handle more walking, standing, slopes or uneven ground than they can comfortably manage at that time, small areas within the tendon and its covering become irritated and less able to cope with the loads they are asked to handle.Each tendon is stressed most when it does its main job: peroneal tendons work harder on uneven ground or when you repeatedly tip towards the outer edge of your foot; the posterior tibial tendon works harder when your heel and ankle roll inwards and your arch collapses; the anterior tibial tendon works harder when lifting the front of the foot, especially on slopes or stairs.How this brace can help here By supporting the heel and ankle in a more neutral position, the brace limits excessive inward or outward roll that repeatedly overstresses these tendons. The heel pad and side panels help keep the foot closer to a central alignment, so the inner and outer tendons are not constantly working at the edge of their range.A more stable base allows you to carry out rehabilitation exercises for these tendons with less risk of flare‑ups from uncontrolled ankle wobble. Many people notice that slopes, uneven ground and simple step‑ups become easier to manage without setting off the same tendon pain each time. The brace does not replace exercise‑based treatment, but it can reduce day‑to‑day irritation while you gradually strengthen and retrain the affected muscles and tendons.Posterior tibial tendon dysfunction and flat feetWhen this usually shows up for you When the tendon that helps support the inner arch is struggling, you may notice that there is pain or aching along the inside of your ankle and into the arch, especially after being on your feet for some time. Your foot may seem to roll inwards more when you stand or walk, the arch can look flatter than it used to, particularly when you are standing, and longer walks or standing on hard floors may leave the inner ankle and lower leg feeling tired and sore.What is happening in the tendon and arch The posterior tibial tendon helps support the inner arch of your foot and prevents the heel and ankle from rolling too far inwards. As the tendon weakens or becomes damaged, it cannot support the arch as effectively. The heel begins to tip inwards and the arch flattens more when you are standing, and weight shifts towards the inner side of the foot.In earlier stages, the arch may look flatter when you are on your feet but reappear when you sit or stand on tiptoe, which is known as a flexible flatfoot. Over time, if strain continues, the flattening can become more fixed, with less change when you come off your feet, and this altered alignment can change how forces pass through the ankle, knee and hip.How this brace can help here The brace supports the inner side of your ankle and the heel.The rigid inner side panel and splint help limit how far your heel and ankle roll inwards with each step. The heel pad provides a more level, supported platform for the back of your foot. This gives any in‑shoe support such as insoles and targeted exercises a more stable base to work from.In earlier stages, this can allow you to stand and walk for longer before the inner ankle and arch start to ache. By keeping the heel more upright, the brace can reduce some of the continual strain on the posterior tibial tendon and inner arch structures during walking and standing. It is most effective when used alongside a tailored exercise programme and any in‑shoe supports or footwear advice you have been given.Osteochondral problems and cuboid syndromeWhen this usually shows up for you Problems affecting specific joint surfaces or small bones in the ankle and midfoot may cause sharp, localised pain with particular movements such as twisting the ankle, turning quickly, or pushing off to the side. There may be a sensation of catching, locking, or a sudden stab in certain positions, and weight‑bearing on a particular part of the foot can feel unreliable.Often, straight‑ahead walking on flat ground may be fairly comfortable, but specific movements, such as cutting to the side, walking on a sloping edge, or pushing off strongly in one direction, provoke the pain.What is happening in the joint surfaces In osteochondral issues around the ankle, a small area of the joint surface and underlying bone may be damaged. Certain angles or shearing movements press or rub this area more, triggering sharp pain or a catching sensation.In cuboid syndrome, the cuboid, a small bone on the outer side of the midfoot that helps form part of the outer arch, can become slightly misaligned or irritated. Movements that load the outer edge of the foot or twist through the midfoot, such as pushing off sideways or landing awkwardly on the outer border of the foot, can aggravate it.How this brace can help here By stabilising your ankle and heel, the brace reduces extreme twisting and side‑to‑side movements that are most likely to stress these specific areas. It encourages a more even distribution of load across the ankle and midfoot during everyday walking, and the cushioned heel pad helps soften impact as weight comes onto the foot.This does not replace targeted treatment from a specialist, but it can reduce the number of sharp, provocative movements in daily life while other therapies do their work. Many people notice fewer sudden, sharp stabs when turning or pushing off to the side once the ankle and heel are better controlled.Drop foot (supportive role at the ankle)When this usually shows up for you With drop foot, lifting the front of the foot is difficult or impossible. The toes may catch or drag on the ground, especially on carpets or uneven surfaces, and the foot may slap down more heavily when you place it. You may find yourself lifting the knee higher than normal or swinging the leg out to the side to clear the toes. These adaptations can make walking more tiring and can feel unstable.What is happening in the leg and ankle Weakness or nerve problems affecting the muscles that lift the front of the foot make it harder to raise the forefoot during the swing phase of walking and increase the risk of stumbles and trips, especially on uneven ground or with changes in surface height. Specialist devices are often used to help lift the front of the foot itself. At the same time, your ankle joint may also feel weak or unstable, and the altered leg swing can add extra side‑to‑side movement at the ankle when the foot lands.How this brace can help here This brace is not designed to lift the front of the foot and does not replace specialist devices that do that job. However, it can provide additional stability around the ankle if there is also weakness or instability in that joint.The side splints and panels limit excessive tilting when the foot lands, which can otherwise be more of a problem when leg swing and foot placement are altered. In this situation, the brace’s job is to steady the ankle once the foot is on the ground, so it is less likely to roll to one side when your toes catch. Under professional guidance, it may be used together with a device that lifts the forefoot during walking, helping to support the ankle while the other device manages the position of the forefoot and toes. Because drop foot usually has complex causes, any use of this brace in that context should be specifically recommended and fitted by a suitable clinician, such as a physiotherapist or orthotist.Bringing it together and next stepsAn ankle that feels painful, weak, or ready to give way at any moment can have a quiet but powerful effect on your confidence and independence. Ligaments may be looser and slower to respond, tendons may be irritated, and the joint surfaces and capsule may be stiff or sensitive after time spent in a cast, boot or simply moving less. All of this can change the way you walk and stand, placing extra strain on other joints and making everyday tasks more tiring.Supporting the ankle from the outside can limit the movements most likely to re‑injure or irritate those tissues, especially sudden inward or outward rolls of the heel and ankle, and can spread forces more evenly through the joint and heel to soften sharp impacts. It also gives you a more secure base from which to rebuild strength, control and trust in your ankle.This rigid, side‑splinted brace, designed by FootReviver and supplied by Nuvoahealth, is built with those goals in mind. The aluminium side splints resist dangerous tilting and help keep your ankle in a safer, more central position. The cushioned heel pad softens impact and supports the back of your foot and heel. The semi‑elastic, padded fabric with smooth edges is made for longer wear, and the two adjustable straps let you set how firm and supportive the brace feels at different stages of recovery and on different days.If your ankle symptoms and experiences match what is described here, and you do not have complex medical issues that need specialist advice first, this brace can be a realistic, practical step towards more stable, less painful movement. At Nuvoahealth, this is the brace many physiotherapists and podiatrists return to when they need firm sideways control but a full boot is no longer appropriate, particularly for ankles that have moved on from a cast but still feel too loose for a soft sleeve.It comes with a 30‑day money‑back guarantee when returned in its original condition, which is there so you can judge for yourself how practical the design is in everyday life. This period is there to help you judge comfort, fit and the sense of support it provides in your usual activities, rather than to promise that all symptoms will fully resolve within that time. Most people know within a few days of typical use whether the brace feels supportive and practical for them.If your symptoms sound similar to the ankle and heel problems described here, this brace is genuinely worth considering, especially if a clinician has advised you to look for a rigid support with side splints and heel cushioning. To move forward, choose the size that best matches your foot and ankle, taking swelling and sock use into account. Think about the parts of your day when your ankle feels least secure – such as longer walks, stairs, time on hard floors, or crowded, uneven environments – and plan to use the brace during those times.If you are unsure whether this brace is right for your specific diagnosis, it is sensible to discuss it with a GP, physiotherapist or podiatrist for guidance. Used in line with their advice, as part of a clear plan, the brace is designed to help you move with more confidence while your ankle continues to heal and adapt.DisclaimerThe information on this page is general guidance for adults and is not a substitute for individual medical advice, diagnosis or treatment. It cannot take account of your full medical history or personal circumstances. If you are unsure whether this brace is suitable for you, or if you have new, complex or worsening symptoms, you should speak to a GP, physiotherapist, podiatrist or another appropriate healthcare professional. No specific outcome can be guaranteed from using this product.
Ankle Supports